Search
- Page Path
- HOME > Search
- Effectiveness of a mobile application for tracking symptoms and enhancing symptom management among breast cancer patients receiving chemotherapy in Bangkok, Thailand: a non-randomized controlled trial
- Duangrat Kaveenuntachai, Supawan Jaiboon, Bualuang Sumdaengrit, Chureeporn Silaguntsuti, Arveewan Vittayatigonnasak, Pornchan Sailamai
- J Korean Acad Nurs 2025;55(2):178-190. Published online May 27, 2025
- DOI: https://doi.org/10.4040/jkan.25011
-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Purpose
This study evaluated the effectiveness of a mobile application in tracking symptoms and improving symptom management and quality of life (QoL) among breast cancer patients undergoing chemotherapy in Thailand.
Methods
A non-randomized controlled trial was used, with 25 participants in the intervention group and 25 in the control group. Research instruments included a demographic data form, the NCI-PRO-CTCAE Items-Thai-Thailand version 1.0, and the European Organization for Research and Treatment of Cancer Quality of Life Core Questionnaire and Breast Cancer-Specific Module.
Results
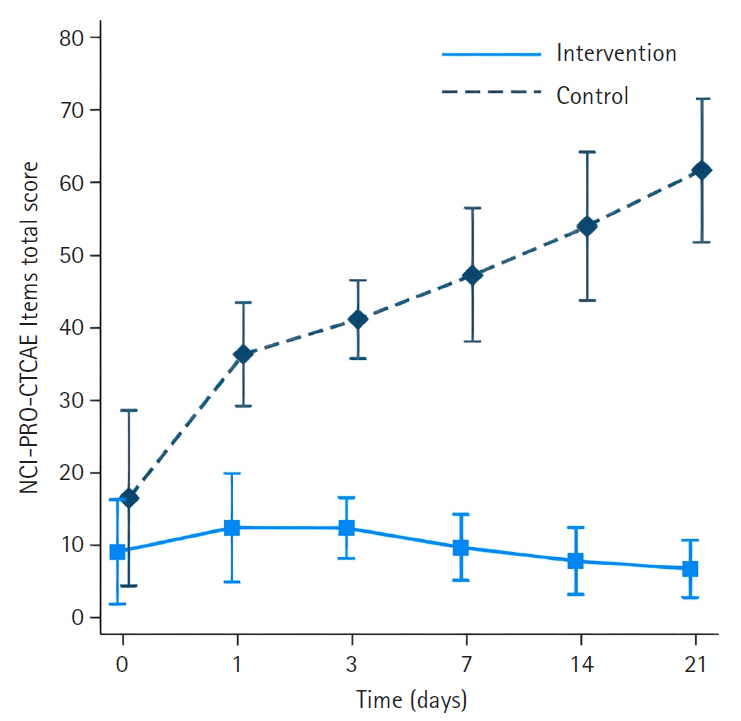
The intervention group had significantly less severe side effects than the control group, with mean differences of –23.33 (95% confidence interval [CI], –27.82 to –18.83) on day 1, –28.18 (95% CI, –33.22 to –23.14) on day 3, –34.63 (95% CI, –40.18 to –29.08) on day 7, –42.56 (95% CI, –48.72 to –36.40) on day 14, and –51.31 (95% CI, –58.13 to –44.48) on day 21 (p<.001 for all). On day 21, participants in the intervention group reported significantly higher scores in the Global Health QoL and Functional Scales compared to the control group (p<.001). Additionally, intervention group participants reported lower scores on the Symptom Scales and higher scores on the Functional Scales than those in the control group (p<.001).
Conclusion
The ChemoPro application helped manage chemotherapy-related symptoms and was associated with improved symptom monitoring and QoL. Nonetheless, the study was limited by a small sample size and restriction to Android users. Future research with larger and more diverse populations is recommended before broader implementation in clinical practice. -
Citations
Citations to this article as recorded by- Effectiveness of a digital health intervention on the supportive care needs and quality of life in Mexican patients with breast cancer: a randomized clinical trial
Saúl Eduardo Contreras-Sánchez, Svetlana V. Doubova, Rocío Grajales-Álvarez, Ricardo Villalobos-Valencia, Abdel Karim Dip-Borunda, José Gustavo Nuñez-Cerrillo, Alma Diana Huerta-López, Álvaro José Montiel-Jarquín, Arturo García-Galicia, Enrique Isay Talam
BMC Cancer.2026;[Epub] CrossRef - Systematic review of patient-reported outcome item libraries in cancer research: an EORTC Quality of Life Group study
Rosemary Peacock, Christopher Bedding, Bonnie Pacheco, Hayat Hamzeh, Claire Piccinin, Alexandra Gilbert
JNCI: Journal of the National Cancer Institute.2026;[Epub] CrossRef
- Effectiveness of a digital health intervention on the supportive care needs and quality of life in Mexican patients with breast cancer: a randomized clinical trial
- 4,793 View
- 252 Download
- 2 Web of Science
- 2 Crossref

- Development and Evaluation of an App-Based Self-Management Program for Exercise Practice of Breast Cancer Survivors: A Non-Randomized Controlled Trial
- Suyoun Maeng, Jungok Yu
- J Korean Acad Nurs 2024;54(2):250-265. Published online May 31, 2024
- DOI: https://doi.org/10.4040/jkan.23119
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study aimed to develop an app-based self-management program based on the transtheoretical model (TTM) for breast cancer survivors’ exercise practice, as well as to investigate the program’s effects on the stage of change for exercise, exercise self-efficacy, exercise decisional balance, exercise amount, and body composition.
Methods
This non-randomized controlled study included 52 participants (26 in each of the experimental and control groups, respectively). An app-based self-management program based on the TTM was conducted with the experimental group for a 12-week period. The program comprised three components: individual coaching for each stage of change for exercise based on TTM, amount of exercise and body composition monitoring, and online self-help meetings.
Results
Compared with the control group, the experimental group had significantly higher stages of change for exercise (p < .001), exercise self-efficacy (p < .001), exercise decisional balance (p = .002), exercise amount (p < .001), and body composition (body weight [p = .006], body mass index [p = .005], and body fat percentage [p = .010]) immediately and four weeks after the intervention.
Conclusion
An appbased self-management program based on the TTM improves exercise behaviors in breast cancer survivors and provides physical benefits. -
Citations
Citations to this article as recorded by- Effects of a mobile health coaching intervention on symptom experience, self-management, and quality of life in breast cancer survivors: A quasi-experimental study
Jin-Hee Park, Sun Hyoung Bae, Yong Sik Jung, Min Hee Hur, Ji Young Kim, Su Jin Jung
Medicine.2025; 104(12): e41894. CrossRef
- Effects of a mobile health coaching intervention on symptom experience, self-management, and quality of life in breast cancer survivors: A quasi-experimental study
- 4,696 View
- 242 Download
- 2 Web of Science
- 1 Crossref

- The Lived Experience of Body Alteration and Body Image with Regard to Immediate Breast Reconstruction among Women with Breast Cancer
- Jeonghee Ahn, Eunyoung E. Suh
- J Korean Acad Nurs 2021;51(2):245-259. Published online April 30, 2021
- DOI: https://doi.org/10.4040/jkan.21028
-
 Abstract
Abstract
 PDF
PDF - Purpose
The purpose of this study was to explore the lived experience of body alteration and body image with regard to immediate breast reconstruction among women with breast cancer.
Methods
Data were collected from July to December 2020 through individual in-depth interviews with 15 women who had undergone immediate breast reconstruction due to breast cancer. Verbatim transcripts were analyzed using Colaizzi’s phenomenological analysis.
Results
The following four theme clusters emerged. First, “revalued meaning of breasts due to cancer” illustrated the fact that cancer removal surgery brought the participants to reconsider the meaning of their breasts. Second, “had no choice but breast reconstruction” demonstrated the participants’ decision-making process of not wanting to lose breasts. Third, “unsatisfied breasts despite reconstruction” portrayed the distress due to the unexpected surgical outcomes. Finally, “restarted everyday routines with the altered body” described the healing process of the participants by accepting their changed body.
Conclusion
In Korea, where family-centeredness and fidelity are highly valued, women perceived their breasts not only as a symbol of femininity but as the mediator connecting the self to family. Despite the distress related to imperfect breasts, the participants were thankful for their reconstructed breasts. Breast reconstruction helped them return to daily life as the psychological trauma of breast cancer was healed. The participants rebuilt their body image by accepting their scarred new body. This may allow health professionals to provide constructive and culturally appropriate counseling in advance by providing insight into women’s perception of their body image with regard to breast reconstruction. -
Citations
Citations to this article as recorded by- A systematic review and meta−analysis on the prepectoral and partial subpectoral immediate single−stage Implant-Based Breast Reconstruction Using ADM
Tingjian Zhang, Yuyao Liu, Liang Huang, Qiang Zhang, Ying Li, Lingyan Du, Xueyun Zhao
Frontiers in Oncology.2026;[Epub] CrossRef - Mental health in female breast cancer survivors post-mastectomy: A structural model based on Roy's adaptation model
Hyeng Sook Yoon, Eunjung Ryu
Asia-Pacific Journal of Oncology Nursing.2025; 12: 100820. CrossRef - Categorising Subjective Perceptions of Middle-Aged Breast Cancer Patients Using Q Methodology
Min-Jeung Shim, Song-Yi Lee, Oh-Sun Ha
Healthcare.2024; 12(18): 1873. CrossRef - Body Acceptance Scale for Women with Breast Cancer: Development and Validation of a Measurement
Jeonghee Ahn, Eunyoung E. Suh
Seminars in Oncology Nursing.2023; 39(5): 151486. CrossRef - Influence of body image on quality of life in breast cancer patients undergoing breast reconstruction: Mediating of self‐esteem
Yunhee Jang, Mihyeon Seong, Sohyune Sok
Journal of Clinical Nursing.2023; 32(17-18): 6366. CrossRef - Body acceptance in women with breast cancer: A concept analysis using a hybrid model
Jeonghee Ahn, Eunyoung E. Suh
European Journal of Oncology Nursing.2023; 62: 102269. CrossRef - A systematic review and meta-analysis on the prepectoral single-stage breast reconstruction
Jiameng Liu, Xiaobin Zheng, Shunguo Lin, Hui Han, Chunsen Xu
Supportive Care in Cancer.2022; 30(7): 5659. CrossRef
- A systematic review and meta−analysis on the prepectoral and partial subpectoral immediate single−stage Implant-Based Breast Reconstruction Using ADM
- 3,283 View
- 101 Download
- 8 Web of Science
- 7 Crossref

- The Effects of Utilizing Smartphone Application Peer Support on Health Behavior and Body Mass Index among Breast Cancer Survivors
- Gaeun Park, Haejung Lee, Hyun Yul Kim
- J Korean Acad Nurs 2019;49(5):550-561. Published online January 15, 2019
- DOI: https://doi.org/10.4040/jkan.2019.49.5.550
-
 Abstract
Abstract
 PDF
PDF Abstract Purpose This study aimed to identify the effects of utilizing Smartphone Application Peer Support (SAPS) on health behavior and body mass index (BMI) among overweight or obese breast cancer survivors (BCS).
Methods A nonequivalent control group with a non-synchronized design was utilized and 36 participants (experimental group 14, control group 22) were recruited from August 2017 to September 2018. Participants were 40~65 years old, overweight or obese, had completed primary cancer treatment within the 12 months prior to the study, and had not done regular exercise during the last 6 months. The 3-month SAPS consisted of exercise and diet education (once p/2 weeks), peer support (once p/week), and self-monitoring using smartphone applications (5 times p/week). All participants underwent assessments at baseline, right after SAPS, and at 3 months after SAPS. Data were analyzed using repeated measures ANOVA.
Results At the completion of SAPS significant differences were found between groups in motivation for exercise (t=-3.24,
p =.005), physical activity (t=-4.15,p <.001), total calorie intake (t=3.42,p =.002), calories from fat (t=-3.01,p =.005), intake of vegetables (t=-2.83,p =.008), and BMI (t=5.21,p <.001). Significant differences in BMI (t=4.13,p <.001) remained up to 3 months after SAPS completion. No significant differences was shown between groups in self-efficacy for exercise, either immediately after or 3 months after SAPS.Conclusion The SAPS has the potential to improve motivation for exercise, health behavior, and BMI of BCS. However, special efforts are required to encourage participants to complete the intervention and maintain long-term effects for future trials.
-
Citations
Citations to this article as recorded by- EHealth intervention for quality of life in long-term breast cancer survivors: randomized controlled trial
Gustavo Adolfo Pimentel-Parra, Nelia Soto-Ruiz, Paula Escalada-Hernández, Leticia San Martín-Rodríguez, Cristina García-Vivar
JNCI: Journal of the National Cancer Institute.2026;[Epub] CrossRef - Efficacy of Mobile App–Based Dietary Interventions Among Cancer Survivors: Systematic Review and Meta-Analysis
Krista Ching Wai Chung, Naomi Takemura, Wendy Wing Tak Lam, Mandy Man Ho, Antoinette Marie Lee, Wynnie Yuen Yee Chan, Daniel Yee Tak Fong
JMIR mHealth and uHealth.2025; 13: e65505. CrossRef - Development and Evaluation of an App-Based Self-Management Program for Exercise Practice of Breast Cancer Survivors: A Non-Randomized Controlled Trial
Suyoun Maeng, Jungok Yu
Journal of Korean Academy of Nursing.2024; 54(2): 250. CrossRef - Effects of an integrated lifestyle intervention for overweight and obese breast cancer survivors: A quasi-experimental study
Su Jin Seo, Ju-Hee Nho
European Journal of Oncology Nursing.2024; 73: 102714. CrossRef - User evaluation of a mobile education application for the management of metabolic syndrome among cancer survivors
Ji-Su Kim, Minhae Kim, Yeji Seo
European Journal of Oncology Nursing.2023; 63: 102276. CrossRef - Effectiveness of Digital Health on the Quality of Life of Long-Term Breast Cancer Survivors: A Systematic Review
Gustavo Adolfo Pimentel-Parra, M. Nelia Soto-Ruiz, Leticia San Martín-Rodríguez, Paula Escalada-Hernández, Cristina García-Vivar
Seminars in Oncology Nursing.2023; 39(4): 151418. CrossRef - Effectiveness of a virtual reality application‐based education programme on patient safety management for nursing students: A pre‐test–post‐test study
Jae Woo Oh, Ji Eun Kim
Nursing Open.2023; 10(12): 7622. CrossRef - Effects of smart-care services program for breast cancer survivors
Bok Yae Chung, Sung Jung Hong
The Journal of Korean Academic Society of Nursing Education.2021; 27(2): 95. CrossRef - The development of a lifestyle modification mobile application, “Health for You” for overweight and obese breast cancer survivors in Korea
Su-Jin Seo, Ju-Hee Nho, Youngsam Park
Korean Journal of Women Health Nursing.2021; 27(3): 243. CrossRef - Peer‐supported lifestyle interventions on body weight, energy intake, and physical activity in adults: A systematic review and meta‐analysis
Siew Lim, Wai Kit Lee, Andy Tan, Mingling Chen, Chau Thien Tay, Surbhi Sood, Stephanie Pirotta, Lisa J. Moran, Meena Daivadanam, Ljoudmila Busija, Helen Skouteris, Mamaru A. Awoke, Briony Hill
Obesity Reviews.2021;[Epub] CrossRef - Application and evaluation of mobile nutrition management service for breast cancer patients
Ji Hee Choi, Seon-Joo Park, Hee Kwon, Hae-Jeung Lee
Journal of Nutrition and Health.2020; 53(1): 83. CrossRef
- EHealth intervention for quality of life in long-term breast cancer survivors: randomized controlled trial
- 1,767 View
- 30 Download
- 10 Web of Science
- 11 Crossref

- A Structural Model for Chemotherapy Related Cognitive Impairment and Quality of Life in Breast Cancer Patients
- Jung Ran Lee, Pok Ja Oh
- J Korean Acad Nurs 2019;49(4):375-385. Published online January 15, 2019
- DOI: https://doi.org/10.4040/jkan.2019.49.4.375
-
 Abstract
Abstract
 PDF
PDF Abstract Purpose This study aimed to develop and test a structural model for chemotherapy-related cognitive impairment of breast cancer patients based on a literature review and Hess and Insel's chemotherapy-related cognitive change model.
Methods The Participants consisted of 250 patients who were ≥19 years of age. The assessment tools included the Menopause Rating Scale, Symptom Experience Scale, Hospital Anxiety and Depression Scale, Everyday Cognition, and Functional Assessment of Cancer Therapy-Breast Cancer. Data were analyzed using the SPSS 21.0 and AMOS 21.0 programs.
Results The modified model was a good fit for the data. The model fit indices were χ 2=423.18 (
p <.001), χ 2/df=3.38, CFI=.91, NFI=.91, TLI=.89, SRMR=.05, RMSEA=.09, and AIC=515.18. Chemotherapy-related cognitive impairment was directly influenced by menopausal symptoms (β=.38,p =.002), depression and anxiety (β=.25,p =.002), and symptom experiences (β=.19,p =.012). These predictors explained 47.7% of the variance in chemotherapy-related cognitive impairment. Depression and anxiety mediated the relations among menopausal symptoms, symptom experiences, and with chemotherapy related cognitive impairment. Depression and anxiety (β=-.51,p =.001), symptom experiences (β=-.27,p =.001), menopausal symptoms (β=-.22,p =.008), and chemotherapy-related cognitive impairment (β=-.15,p =.024) had direct effects on the quality of life and these variables explained 91.3%.Conclusion These results suggest that chemotherapy-related toxicity is highly associated with cognitive decline and quality of life in women with breast cancer. Depression and anxiety increased vulnerability to cognitive impairment after chemotherapy. Nursing intervention is needed to relieve chemotherapy-related toxicity and psychological factor as well as cognitive decline for quality of life in patients undergoing chemotherapy.
-
Citations
Citations to this article as recorded by- Analysis of Breast Cancer Nursing Education Content and Educational needs for Breast Cancer Patient Nursing Perceived by Nurses
Young-Hee Je, Kyoung-Ah Kang
Asian Oncology Nursing.2025; 25(1): 1. CrossRef - Impact of social support on cognitive function in patients with breast cancer undergoing chemotherapy: The chain-mediating role of fatigue and depression
Yuanqi Ding, Qingmei Huang, Fulei Wu, Yang Yang, Ling Wang, Xuqian Zong, Xiaoyan Yu, Changrong Yuan
Asia-Pacific Journal of Oncology Nursing.2025; 12: 100743. CrossRef - Factors Influencing Oncofertility in Gynecological Cancer Patients: Application of Mixed Methods Study
Minji Kim, Juyoung Ha
Journal of Korean Academy of Nursing.2024; 54(3): 418. CrossRef - Relationships Between Chemotherapy-Related Cognitive Impairment, Self-Care Ability, and Quality of Life in Breast Cancer Survivors: A Cross-Sectional Study
Nan Wu, Ze Luan, Zijun Zhou, He Wang, Shiyuan Du, Yulu Chen, Xinxin Wang, Jiong Li, Xin Peng
Seminars in Oncology Nursing.2024; 40(5): 151690. CrossRef - Effects of different exercise interventions on chemotherapy-related cognitive impairment in patients with breast cancer: a study protocol for systematic review and network meta-analysis
Yu Dong, Hao Huang, Aiping Wang
BMJ Open.2024; 14(4): e078934. CrossRef - Factors Associated with Self-reported Memory Problems of Adult Cancer Survivors Based on the Korea National Health and Nutrition Examination Survey 2019
Sangjin Ko
Journal of Health Informatics and Statistics.2023; 48(1): 51. CrossRef - Impact of nonpharmacological interventions on cognitive impairment in women with breast cancer: A systematic review and meta-analysis
Jin-Hee Park, Su Jin Jung, Lena J. Lee, Junghyun Rhu, Sun Hyoung Bae
Asia-Pacific Journal of Oncology Nursing.2023; 10(4): 100212. CrossRef - Impact of discriminant factors on the comfort-care of nurses caring for trans-arterial chemoembolisation patients
Myoung Soo Kim, Ju-Yeon Uhm
Supportive Care in Cancer.2022; 30(9): 7773. CrossRef - Brain morphological alterations and their correlation to tumor differentiation and duration in patients with lung cancer after platinum chemotherapy
Pin Lv, Guolin Ma, Wenqian Chen, Renyuan Liu, Xiaoyan Xin, Jiaming Lu, Shu Su, Ming Li, ShangWen Yang, Yiming Ma, Ping Rong, Ningyu Dong, Qian Chen, Xin Zhang, Xiaowei Han, Bing Zhang
Frontiers in Oncology.2022;[Epub] CrossRef - The Influence of Rehabilitation on Quality of Life in Breast Cancer Survivors: A Clinical Study
Teresa Paolucci, Aristide Saggino, Francesco Agostini, Marco Paoloni, Andrea Bernetti, Massimiliano Mangone, Valter Santilli, Raoul Saggini, Marco Tommasi
International Journal of Environmental Research and Public Health.2021; 18(16): 8585. CrossRef
- Analysis of Breast Cancer Nursing Education Content and Educational needs for Breast Cancer Patient Nursing Perceived by Nurses
- 2,036 View
- 27 Download
- 10 Web of Science
- 10 Crossref

- Psychoeducational Approach to Distress Management of Newly Diagnosed Patients with Breast Cancer
- Jin-Hee Park, Mison Chun, Yong Sik Jung, Sun Hyoung Bae, Young-Mi Jung
- J Korean Acad Nurs 2018;48(6):669-678. Published online January 15, 2018
- DOI: https://doi.org/10.4040/jkan.2018.48.6.669
-
 Abstract
Abstract
 PDF
PDF Abstract Purpose The purpose of this study was to examine the effects of integrated psychoeducational program for distress management of newly diagnosed patients with breast cancer.
Methods A quasi-experimental trial was conducted. The participants consisted of 47 female patients with breast cancer assigned to an intervention group (n=25) and control group (n=22). The intervention group participated in integrated psychoeducational program, consisting of individual face-to-face education and telephone-delivered health-coaching sessions. Data were collected at three time points: pre-intervention (T1), post-intervention (T2), and 6-month follow-up (T3). Study instruments were Distress thermometer, Supportive Care Needs Survey Short Form 34 and Functional Assessment of Cancer Therapy-Breast.
Results Compared with the control group, breast cancer patients in the intervention group reported lower distress and supportive care needs than the control group. The intervention group reported higher quality of life (QOL) overall and higher emotional well-being than the control group.
Conclusion These findings indicate that the integrated psychoeducational program is an effective intervention for reducing distress and supportive care needs and increasing QOL of newly diagnosed patients with breast cancer. Oncology nurses need to provide psychoeducational intervention to support patients with breast cancer in managing their distress and helping them adjust to their life.
-
Citations
Citations to this article as recorded by- Nurse Coaching in Oncology Care to Reduce Stress: A Systematic Review and Meta-Analysis
Elsa Vitale, Lorenza Maistrello, Karen Avino, Giuseppe Colonna, Ivan Rubbi, Roberto Lupo
Healthcare.2026; 14(7): 840. CrossRef - Breast Cancer Nursing Competencies for General Nurses Caring For Breast Cancer Patients: A Delphi Study
Young-Hee Je, Hee-Jung Kang
Asian Oncology Nursing.2026; 26(1): 1. CrossRef - Analysis of Breast Cancer Nursing Education Content and Educational needs for Breast Cancer Patient Nursing Perceived by Nurses
Young-Hee Je, Kyoung-Ah Kang
Asian Oncology Nursing.2025; 25(1): 1. CrossRef - Effectiveness of a Tailored Psychoeducational Intervention for Patients With Advanced Cancer in Indonesia: A Randomized Controlled Trial
Nurul Huda, Made Satya Nugraha Gautama, Wan Nishfa Dewi, Agung Waluyo, Hsiu Ju Chang, Malissa Kay Shaw
Journal of Nursing Scholarship.2025; 57(5): 848. CrossRef - Evidence on the benefits of mind-body Qigong exercise in women with breast cancer
Michel Marcos Dalmedico, Jackson Adriano Canavarro Ribeiro, Juliana Londero Silva Avila, Prisley Pereira de Oliveira, Paula Karina Hembecker, Sergio Ossamu Ioshii
Fisioterapia em Movimento.2025;[Epub] CrossRef - Psychological Distress and Influencing Factors in Newly Diagnosed Patients with Breast Cancer: A Cross-Sectional Study
Jin-Hee Park, Yong Sik Jung, Min Hee Hur, Yu Jin Jeong
Korean Journal of Adult Nursing.2024; 36(4): 311. CrossRef - Effects of Psychosocial Interventions for Patients with Breast Cancer: A Meta-analysis
Kyu-Sic Hwang, Kuy-Haeng Lee, Chan-Mo Yang, Hye-Jin Lee, Sang-Yeol Lee
Clinical Psychopharmacology and Neuroscience.2023; 21(1): 118. CrossRef - The development of a lifestyle modification mobile application, “Health for You” for overweight and obese breast cancer survivors in Korea
Su-Jin Seo, Ju-Hee Nho, Youngsam Park
Korean Journal of Women Health Nursing.2021; 27(3): 243. CrossRef - Development and Effect of the Integrated Health Promotion Program for Cancer Survivors Living at Home
Hee Sang Yoon, Eun A Hwang
Journal of Korean Academy of Community Health Nursing.2021; 32(1): 51. CrossRef - Adjustment to life with metastatic cancer through psychodrama group therapy: A qualitative study in Turkey
Songül Kamışlı, Bahar Gökler
Perspectives in Psychiatric Care.2021; 57(2): 488. CrossRef - Integration of longitudinal psychoeducation programmes during the phases of diagnosis, management and survivorship of breast cancer patients: A narrative review
Athena Michaelides, Constantina Constantinou
Journal of Cancer Policy.2020; 23: 100214. CrossRef - Quality of Life in Patients Undergoing Mastectomy for Breast Cancer
Kavitha Konnakkaparambil Ramakrishnan, Sreekumar Damodaran
Journal of Evidence Based Medicine and Healthcare.2020; 7(28): 1368. CrossRef - Mediating and Moderating Factors of Adherence to Nutrition and Physical Activity Guidelines, Breastfeeding Experience, and Spousal Support on the Relationship between Stress and Quality of Life in Breast Cancer Survivors
Nam Mi Kang, Won-Ho Hahn, Suyeon Park, Jung Eun Lee, Young Bum Yoo, Chung Ja Ryoo
International Journal of Environmental Research and Public Health.2020; 17(20): 7532. CrossRef - Uncertainty and unmet care needs before and after surgery in patients with gastric cancer: A survey study
Ji Yea Lee, Yeonsoo Jang, Sanghee Kim, Woo Jin Hyung
Nursing & Health Sciences.2020; 22(2): 427. CrossRef - Effects of Different Exercise Interventions on Quality of Life in Breast Cancer Patients: A Randomized Controlled Trial
Tetiana Odynets, Yuriy Briskin, Valentina Todorova
Integrative Cancer Therapies.2019;[Epub] CrossRef
- Nurse Coaching in Oncology Care to Reduce Stress: A Systematic Review and Meta-Analysis
- 2,093 View
- 48 Download
- 15 Crossref

- Symptom Distress and Coping in Young Korean Breast Cancer Survivors: The Mediating Effects of Social Support and Resilience
- Ji Hyun Lee, Hye Young Kim
- J Korean Acad Nurs 2018;48(2):241-253. Published online January 15, 2018
- DOI: https://doi.org/10.4040/jkan.2018.48.2.241
-
 Abstract
Abstract
 PDF
PDF Abstract Purpose The purpose of this study was to test the mediating effect of social support and resilience on the relationship between symptom distress and coping in young Korean breast cancer survivors.
Methods A purposive sample of 209 young breast-cancer survivors (mean age 39.9) was recruited for a cross-sectional survey, and the data were collected between June and October 2015. The instruments used in this study were the Memorial Symptom Assessment Scale-Short Form, the Multidimensional Scale of Perceived Social Support, 10-item Connor-Davidson Resilience Scale, and Cancer Coping Questionnaire. The collected data were then analyzed using the SPSS 23.0 and AMOS 23.0 programs.
Results Symptom distress was found to have a significant indirect effect on coping (beta=-.32,
p =.002), but not a significant direct effect (beta=.06,p =.577). Additionally, based on the values obtained for the squared multiple correlation, symptom distress, social support, and resilience were found to explain 46.4% of the total variance of coping.Conclusion Based on the results of this study, it can be suggested that in order to enhance young breast cancer survivors’ ability to cope with the distress they commonly feel, intervention methods that strengthen resilience and provide social support should be developed and made available to them.
-
Citations
Citations to this article as recorded by- Sexual well-being in cancer care services: the role of body image and coping strategies
Judith Partouche-Sebban, Saeedeh Rezaee Vessal, Youssef Souak, Aymen Ammari, Alain Toledano
Journal of Services Marketing.2026; : 1. CrossRef - How Online Patient-Provider Communication Alleviates Psychological Distress Among Patients with Chronic Diseases: The Role of Perceived Patient-Centered Communication and Adaptive Coping Strategies
Bingqing Ling, Yu Zheng
Health Communication.2025; 40(8): 1559. CrossRef - Factors Associated With Not Returning to Work Among Breast Cancer Survivors
Leni Merdawati, Hui-Chen Lin, Chieh-Hsin Pan, Hui-Chuan Huang
Workplace Health & Safety.2025; 73(5): 216. CrossRef - Factors affecting resilience among young breast cancer survivors: A cross-sectional study
Hye Young Min, Yoonjung Kim, Hae Jeong An
European Journal of Oncology Nursing.2025; 75: 102837. CrossRef - Latent classes of health‐promoting lifestyle in breast cancer patients undergoing chemotherapy in China: A cross‐sectional survey
Meixuan Song, Qiuyao He, Juan Yang, Jinyu Zhang
Nursing Open.2024;[Epub] CrossRef - Postmastectomy Pain Syndrome: A Narrative Review
Sajad Ahmad Salati, Lamees Alsulaim, Mariyyah H Alharbi, Norah H Alharbi, Thana M Alsenaid, Shoug A Alaodah, Abdulsalam S Alsuhaibani, Khalid A Albaqami
Cureus.2023;[Epub] CrossRef - Effects of the CALM intervention on resilience in Chinese patients with early breast cancer: a randomized trial
Shaochun Liu, Runze Huang, Anlong Li, Sheng Yu, Senbang Yao, Jian Xu, Lingxue Tang, Wen Li, Chen Gan, Huaidong Cheng
Journal of Cancer Research and Clinical Oncology.2023; 149(20): 18005. CrossRef - Perceived social support and depressive symptoms in Chinese patients with ovarian cancer and the mediating role of resilience:a cross-sectional study
Xiaoyan Pang, Fangmei Li, Lei Dou, Yichang Tian, Yi Zhang
Current Psychology.2023; 42(24): 20485. CrossRef - Resilience-related Breast Cancer: A Concept Analysis
Fitria Endah Janitra, Nur Aini, Anggi Lukman Wicaksana
Nurse Media Journal of Nursing.2023; 13(1): 31. CrossRef - Factors influencing the coping strategies of liver cancer patients undergoing transarterial chemoembolization
Su‐Chih Chen, Shu‐Fang Wu, Tsae‐Jyy Wang, John Rosenberg, Yu‐Ying Lu, Shu‐Yuan Liang
International Journal of Nursing Practice.2022;[Epub] CrossRef - Perceived social support and coping style as mediators between resilience and health-related quality of life in women newly diagnosed with breast cancer: a cross-sectional study
Kaina Zhou, Fan Ning, Xiao Wang, Wen Wang, Dongfang Han, Xiaomei Li
BMC Women's Health.2022;[Epub] CrossRef - Determinants of quality of life in women immediately following the completion of primary treatment of breast cancer: A cross-sectional study
Jin-Hee Park, Yong Sik Jung, Ji Young Kim, Sun Hyoung Bae, Ka Ming Chow
PLOS ONE.2021; 16(10): e0258447. CrossRef - A Mobile Healing Program Using Virtual Reality for Sexual Violence Survivors: A Randomized Controlled Pilot Study
Mi‐ran Lee, Chiyoung Cha
Worldviews on Evidence-Based Nursing.2021; 18(1): 50. CrossRef - Factors related to the resilience and mental health of adult cancer patients: a systematic review
Saori Tamura, Kumi Suzuki, Yuri Ito, Akiko Fukawa
Supportive Care in Cancer.2021; 29(7): 3471. CrossRef - Resilience in women with breast cancer: A systematic review
Ibane Aizpurua-Perez, Joana Perez-Tejada
European Journal of Oncology Nursing.2020; 49: 101854. CrossRef - Individual resilience in adult cancer care: A concept analysis
Dan Luo, Manuela Eicher, Kate White
International Journal of Nursing Studies.2020; 102: 103467. CrossRef - Relationship between cancer stigma, social support, coping strategies and psychosocial adjustment among breast cancer survivors
No Eul Kang, Hye Young Kim, Ji Young Kim, Sung Reul Kim
Journal of Clinical Nursing.2020; 29(21-22): 4368. CrossRef - Effects of cyclic adjustment training delivered via a mobile device on psychological resilience, depression, and anxiety in Chinese post-surgical breast cancer patients
Kaina Zhou, Jin Li, Xiaomei Li
Breast Cancer Research and Treatment.2019; 178(1): 95. CrossRef
- Sexual well-being in cancer care services: the role of body image and coping strategies
- 2,343 View
- 30 Download
- 18 Crossref

- Impact of Uncertainty on the Quality of Life of Young Breast Cancer Patients: Focusing on Mediating Effect of Marital Intimacy
- Yeong Kyong Oh, Seon Young Hwang
- J Korean Acad Nurs 2018;48(1):50-58. Published online January 15, 2018
- DOI: https://doi.org/10.4040/jkan.2018.48.1.50
-
 Abstract
Abstract
 PDF
PDF Abstract Purpose The purpose of this study was to examine the mediating effect of marital intimacy on the impact of uncertainty on the quality of life (QoL) of young breast cancer patients.
Methods This study used a pathway analysis with 154 young breast cancer cases in their early diagnosis stage at a medical center in Korea. Data were collected from November 2016 to February 2017 and analyzed using correlation analysis and pathway analysis.
Results Uncertainty, marital intimacy, and 4 sub-scales of QoL showed a significant correlation. Marital intimacy was directly affected by uncertainty (b=-.39,
p =.013) and 4 sub-scales of QoL were also affected by uncertainty. Among the 4 sub-scales of QoL, physical well-being (PWB) (b=.17,p =.026), social well-being (SWB) (b=.49,p =.010), and functional well-being (FWB) (b=.38,p =.009) were affected by marital intimacy but emotional well-being (EWB) was not affected by it. The mediating effect of marital intimacy on the impact of uncertainty on QoL was confirmed. Marital intimacy showed a significant indirect effect on PWB (b=-.07,p =.024), SWB (b=-.19,p =.008), and FWB (b=-.15,p =.005), and it means that marital intimacy has a partial mediating effect on the impact of uncertainty on PWB, SWB, and FWB.Conclusion Effects of uncertainty on QoL was mediated by marital intimacy of young breast cancer patients in their early diagnosis stage. It suggests that marital intimacy needs to be considered in providing nursing intervention for young breast cancer patients.
-
Citations
Citations to this article as recorded by- Sexual well-being in cancer care services: the role of body image and coping strategies
Judith Partouche-Sebban, Saeedeh Rezaee Vessal, Youssef Souak, Aymen Ammari, Alain Toledano
Journal of Services Marketing.2026; : 1. CrossRef - Incertidumbre en mujeres diagnosticadas con cáncer de mama: estudio transversal
Rosa Herminia Pastuña-Doicela, Olivia Inés Sanhueza-Alvarado
Escola Anna Nery.2024;[Epub] CrossRef - Uncertainty in women diagnosed with breast cancer: a cross-sectional study
Rosa Herminia Pastuña-Doicela, Olivia Inés Sanhueza-Alvarado
Escola Anna Nery.2024;[Epub] CrossRef - Body change stress, sexual function, and marital intimacy in korean patients with breast cancer receiving adjuvant chemotherapy: A cross-sectional study
Hyesoon Lee, Hyeon Gyeong Yoon
Asia-Pacific Journal of Oncology Nursing.2023; 10(5): 100228. CrossRef - Factors influencing the supportive care needs of female patients with genital cancer in South Korea
Yu-Jung Son, Keum-Hee Nam, JaeLan Shim
Medicine.2023; 102(51): e36650. CrossRef - An explanatory model of quality of life in high-risk pregnant women in Korea: a structural equation model
Mihyeon Park, Sukhee Ahn
Korean Journal of Women Health Nursing.2023; 29(4): 302. CrossRef - Impacts of Uncertainty and Social Support on the Quality of Life of Breast Cancer Survivors after Chemotherapy: Based on Self-help Group Participants
Hyenam Hwang, Yoonshin Lee
Asian Oncology Nursing.2023; 23(4): 177. CrossRef - A hermeneutic phenomenological study on the disease experience among young women with breast cancer
Jeonghee Ahn, Kyoung-eun Lee
Asia-Pacific Journal of Oncology Nursing.2023; 10(10): 100310. CrossRef - Psychological variables associated with quality of life in patients with head and neck cancer: the role of body image distress
Silvia Cerea, Maria Sansoni, Giovanni Scarzello, Elena Groff, Marta Ghisi
Supportive Care in Cancer.2022; 30(11): 9127. CrossRef - Relationships among sexual function, marital intimacy, type D personality and quality of life in patients with ovarian cancer, with spouses
Ju‐Hee Nho, Sung Reul Kim, Won Ku Choi
European Journal of Cancer Care.2022;[Epub] CrossRef - The Relationships among Social Support, Bowel Function Symptoms and Uncertainty in Rectal Cancer Patients
Kyungmi Lee, Semi Lim
Journal of Korean Academy of Fundamentals of Nursing.2021; 28(4): 421. CrossRef - The development of a lifestyle modification mobile application, “Health for You” for overweight and obese breast cancer survivors in Korea
Su-Jin Seo, Ju-Hee Nho, Youngsam Park
Korean Journal of Women Health Nursing.2021; 27(3): 243. CrossRef - Mediating and Moderating Factors of Adherence to Nutrition and Physical Activity Guidelines, Breastfeeding Experience, and Spousal Support on the Relationship between Stress and Quality of Life in Breast Cancer Survivors
Nam Mi Kang, Won-Ho Hahn, Suyeon Park, Jung Eun Lee, Young Bum Yoo, Chung Ja Ryoo
International Journal of Environmental Research and Public Health.2020; 17(20): 7532. CrossRef - Effects of uncertainty and spousal support on infertility-related quality of life in women undergoing assisted reproductive technologies
Hye Shin Lee, Sunjoo Boo, Jeong-Ah Ahn, Ju-Eun Song
Korean Journal of Women Health Nursing.2020; 26(1): 72. CrossRef - Impact of Psycho-Social Factors on Fatigue among Breast Cancer Patients Who Are Currently Undergoing Radiotherapy
Hyesun Park, Kisook Kim
International Journal of Environmental Research and Public Health.2020; 17(17): 6092. CrossRef - Health care Utilization of Cancer patient Women at Nursing Hospital
Hye-Sun Park, Kyung-Sook Park
Journal of Digital Contents Society.2018; 19(11): 2139. CrossRef
- Sexual well-being in cancer care services: the role of body image and coping strategies
- 1,606 View
- 14 Download
- 16 Crossref

- Effects of Educational Program of Manual Lymph Massage on the Arm Functioning and the Quality of Life in Breast Cancer Patients
- Eun Sook Lee, Sung Hyo Kim, Sun Mi Kim, Jeong Ju Sun
- Journal of Korean Academy of Nursing 2005;35(7):1390-1400. Published online March 28, 2017
- DOI: https://doi.org/10.4040/jkan.2005.35.7.1390
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to determine the effect of EPMLM(educational program of manual lymph massage) on the arm functioning and QOL(quality of life) in breast cancer patients with lymphedema.
Method Subjects in the experimental group(n=20) participated in EPMLM for 6 weeks from June to July, 2005. The EPMLM consisted of training of lymph massage for 2 weeks and encourage and support of self-care using lymph massage for 4 weeks. The arm functioning assessed at pre-treatment, 2weeks, and 6weeks using Arm functioning questionnaire. The QOL assessed at pre-treatment and 6 weeks using SF-36. The outcome data of experimental group was compared with control group(n=20). The collected data was analyzed by using SPSS 10.0 statistical program.
Result The arm functioning of experimental group was increased from 2 weeks after(W=.224, p=.011) and statistically differenced with control group at 2 weeks(Z=-2.241, p=.024) and 6 weeks(Z=-2.453, p=.013). Physical function of QOL domain increased in experimental group(Z=-1.162, p=.050), also statistically differenced with control group(Z=-2.182, p= .030) at 6weeks.
Conclusion The results suggest that the educational program of manual lymph massage can improve arm functioning and physical function of QOL domain in breast cancer patients with lymphedema.
-
Citations
Citations to this article as recorded by- Analysis of Domestic Manual Lymph Drainage (MLD)-related Research Trend
Ji-Hyun Mun, Min-Hee Kim
Fashion & Textile Research Journal.2022; 24(5): 636. CrossRef - Changes in Upper Extemity Sensation and the Quality of Life for Patients Following Mastectomy
Suk Jeong Lee, Young Mi Park, Jiyoung Kim
Journal of Korean Oncology Nursing.2011; 11(3): 229. CrossRef
- Analysis of Domestic Manual Lymph Drainage (MLD)-related Research Trend
- 1,019 View
- 5 Download
- 2 Crossref

- Effects of a Comprehensive Rehabilitation Program for Mastectomy Patients
- Ok Hee Cho
- Journal of Korean Academy of Nursing 2004;34(5):809-819. Published online March 28, 2017
- DOI: https://doi.org/10.4040/jkan.2004.34.5.809
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to investigate the effect of a comprehensive rehabilitation program on physical function, immune response, fatigue and quality of life in mastectomy patients.
Method The subjects included fifty-five patients with breast cancer (27 in the control group and 28 in the experimental group). The subjects in the experimental group participated in a comprehensive rehabilitation program for10 weeks, which was composed of 1 session of education, 2 sessions of stress management, 2 sessions of exercise, and 1 session of peer support group activity per week.
Result The results revealed anincrease in shoulder extension, abduction, external rotation, and internal rotation of the affectedupper extremity, and in shoulder extension and abduction of the healthy upper extremity. Also an increase in quality of life and a decrease in fatigue were significantly higher in the experimental group than the control group. However, the results revealed that the natural killer cell ratio of the experimental group increased but there was no significant difference from that of the control group.
Conclusion The 10-week comprehensive rehabilitation program showed a large affirmative effect on physical function, fatigue and quality of life of breast cancer patients after a mastectomy.
-
Citations
Citations to this article as recorded by- The Effect of Comprehensive Care Program for Ovarian Cancer Survivors
Kyung-Hye Hwang, Ok-Hee Cho, Yang-Sook Yoo
Clinical Nursing Research.2016; 25(2): 192. CrossRef - Review of Rehabilitation Programs for Cancer survivors
Jong Hee Han
Journal of the Korea Academia-Industrial cooperation Society.2016; 17(12): 307. CrossRef - Effect of a 12-week walking exercise program on body composition and immune cell count in patients with breast cancer who are undergoing chemotherapy
Ji Jeong Kim, Yun A Shin, Min Hwa Suk
Journal of Exercise Nutrition & Biochemistry.2015; 19(3): 255. CrossRef - Effects of BeHaS Exercise Program on Flexibility, Grip Strength, Stress and Self-esteem in Breast Cancer Survivors
Sun Young Park, Jong Im Kim
Journal of muscle and joint health.2013; 20(3): 171. CrossRef - Relationships among Pain, Upper Extremity Function, and Anxiety in the Breast Cancer Survivors
Jeong-Sun Lim, Jong-Im Kim
Journal of muscle and joint health.2012; 19(1): 37. CrossRef - Effects of Laughter Therapy on Depression, Quality of Life, Resilience and Immune Responses in Breast Cancer Survivors
Eun A Cho, Hyun Ei Oh
Journal of Korean Academy of Nursing.2011; 41(3): 285. CrossRef - Developing a Rehabilitation Model of Breast Cancer Patients Through Literature Review and Hospital Rehabilitation Programs
Bok-Yae Chung, Yu Xu
Asian Nursing Research.2008; 2(1): 55. CrossRef
- The Effect of Comprehensive Care Program for Ovarian Cancer Survivors
- 1,029 View
- 34 Download
- 7 Crossref

- Decision Making Experience on Breast Reconstruction for Women with Breast Cancer
- Myungsun Yi, Woo Joung Joung, Eun Young Park, Eun Jin Kwon, Haejin Kim, Ji Young Seo
- J Korean Acad Nurs 2016;46(6):894-904. Published online December 30, 2016
- DOI: https://doi.org/10.4040/jkan.2016.46.6.894
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to explore decision making experiences of Korean women with breast cancer who underwent breast reconstruction with/after a mastectomy.
Methods Data were collected during 2015-2016 through individual in-depth interviews with 10 women who had both mastectomy and breast reconstruction, and analyzed using phenomenological method to identify essential themes on experiences of making a decision to have breast reconstruction.
Results Five theme clusters emerged. First, “expected loss of sexuality and discovery of autonomy” illustrates various aims of breast reconstruction. Second, “holding tight to the reputation of doctors amid uncertainty” specifies the importance of a trust relationship with their physician despite a lack of information. Third, “family members to step back in position” describes support or opposition from family members in the decision making process. Fourth, “bewilderment due to the paradox of appearance-oriented views” illustrates paradoxical environment, resulting in confusion and anger. Lastly, “decision to be made quickly with limited time to oneself” describes the crazy whirling process of decision making.
Conclusion Findings highlight aims, worries, barriers, and facilitators that women with breast cancer experience when making a decision about breast reconstruction. Deciding on breast reconstruction was not only a burden for women in a state of shock with a diagnosis of breast cancer, but also an opportunity to decide to integrate their body, femininity, and self which might be wounded from a mastectomy. These findings will help oncology professionals provide effective educational counselling before the operation to promote higher satisfaction after the operation.
-
Citations
Citations to this article as recorded by- Mental health in female breast cancer survivors post-mastectomy: A structural model based on Roy's adaptation model
Hyeng Sook Yoon, Eunjung Ryu
Asia-Pacific Journal of Oncology Nursing.2025; 12: 100820. CrossRef - Influence of body image on quality of life in breast cancer patients undergoing breast reconstruction: Mediating of self‐esteem
Yunhee Jang, Mihyeon Seong, Sohyune Sok
Journal of Clinical Nursing.2023; 32(17-18): 6366. CrossRef - Effects of decision aids on breast reconstruction: A systematic review and meta‐analysis of randomised controlled trials
Shu Yang, Lin Yu, Chunmiao Zhang, Mengmeng Xu, Qi Tian, Xuan Cui, Yantong Liu, Shuanghan Yu, Minglu Cao, Wei Zhang
Journal of Clinical Nursing.2023; 32(7-8): 1025. CrossRef - “Struggling to Accept the New Breast as Part of My Body” – The Challenge of Immediate Breast Reconstruction in Women With Breast Cancer
Jeehee Han, Juhye Jin, Sanghee Kim, Dong Won Lee, Sue Kim
Cancer Nursing.2022; 45(4): 262. CrossRef - Do COVID-19–Related Treatment Changes Influence Fear of Cancer Recurrence, Anxiety, and Depression in Breast Cancer Patients?
Soo Yeon Kim, Sue Kim
Cancer Nursing.2022; 45(2): E628. CrossRef - A Decision Tree Model for Breast Reconstruction of Women with Breast Cancer: A Mixed Method Approach
Eun Young Park, Myungsun Yi, Hye Sook Kim, Haejin Kim
International Journal of Environmental Research and Public Health.2021; 18(7): 3579. CrossRef - The Lived Experience of Body Alteration and Body Image with Regard to Immediate Breast Reconstruction among Women with Breast Cancer
Jeonghee Ahn, Eunyoung E Suh
Journal of Korean Academy of Nursing.2021; 51(2): 245. CrossRef - Factors Influencing Quality of Life Among Breast Cancer Patients Following Immediate Breast Reconstruction
A Young Kim, Jeong Hye Kim
Asian Oncology Nursing.2020; 20(1): 1. CrossRef - Korean Translation and Psychometric Evaluation of Korean Version EORTC QLQ-BRECON23
Soo-Kyung Bok, Youngshin Song, Ancho Lim, Hyunsuk Choi, Hyunkyung Shin, Sohyun Jin
International Journal of Environmental Research and Public Health.2020; 17(24): 9163. CrossRef - Operation Experiences of Women with Breast Cancer
Hyeon-Young Kim, Sun Hwa Shin
Journal of Korean Academy of Fundamentals of Nursing.2020; 27(2): 129. CrossRef - “Waiting for breast reconstruction”: An interpretative phenomenological analysis of heterosexual couples’ experiences of mastectomy for breast cancer
Kristopher Lamore, Cécile Flahault, Léonor Fasse, Aurélie Untas
European Journal of Oncology Nursing.2019; 42: 42. CrossRef - Breast reconstruction statistics in Korea from the Big Data Hub of the Health Insurance Review and Assessment Service
Jae-Won Kim, Jun-Ho Lee, Tae-Gon Kim, Yong-Ha Kim, Kyu Jin Chung
Archives of Plastic Surgery.2018; 45(05): 441. CrossRef
- Mental health in female breast cancer survivors post-mastectomy: A structural model based on Roy's adaptation model
- 1,409 View
- 15 Download
- 12 Crossref

- Factors Influencing Posttraumatic Growth in Survivors of Breast Cancer
- Jin-Hee Park, Yong-Sik Jung, Youngmi Jung
- J Korean Acad Nurs 2016;46(3):454-462. Published online June 30, 2016
- DOI: https://doi.org/10.4040/jkan.2016.46.3.454
-
 Abstract
Abstract
 PDF
PDF Purpose Posttraumatic growth (PTG) is defined as 'positive psychological change experienced as a result of a struggle with highly challenging life circumstances'. The purpose of this study was to identify the level of PTG and its correlates in Korean patients with breast cancer.
Methods A sample of 120 participants was recruited from outpatients, who had successfully completed primary treatment of breast cancer at a university hospital., Data were collected from June to December, 2014 using Posttraumatic Growth Inventory, lllness Intrusiveness Rating Scale, Cancer Coping Questionnaire, Revised Life Orientation Test and The Multidimensional Scale of Perceived Social Support.
Results Total score for the PTG was 79.18±17.54 in patients surviving breast cancer. Bivariate analyses indicated that PTG was positively associated with having a religion, perceived social support, greater optimism, cancer coping, and illness intrusiveness. Results of the regression analysis showed that cancer coping (β=.29,
p =.001), optimism (β=0.28,p =.001) and illness intrusiveness (β=0.17,p =.037) were statistically significant in patients' PTG.Conclusion The research findings show that the variables of cancer coping, optimism and illness intrusiveness significantly explain PTG and these psychological variables can be used to provide improvement in PTG for patients with breast cancer
-
Citations
Citations to this article as recorded by- The influence of locus of control, coping strategies and time perspective on post-traumatic growth in survivors with primary breast cancer
Alexandra-Cristina Paunescu, Marina Kvaskoff, Cyrille Delpierre, Lidia Delrieu, Guillemette Jacob, Myriam Pannard, Marie Préau
BMC Psychology.2025;[Epub] CrossRef - Do caregivers of traumatic brain injury survivors experience post-traumatic growth? A mixed-methods study exploring the positive experiences of informal caregivers
Molly Hillyard, Ryan Westley, Jade Kettlewell, Melissa Brunner
Brain Impairment.2025;[Epub] CrossRef - Post-traumatic growth and its influencing factors in first-episode stroke patients: a cross-sectional study
Minli Hu, Yue Ban, Zhihui Li, Yu He, Liping Deng, Xiaohua Xie
BMC Psychology.2025;[Epub] CrossRef - Factors Influencing Resilience in Patients with Multiple Myeloma: A Cross-Sectional Study
Hae-Lyeon Jeon, Hye-Ah Yeom
Korean Journal of Adult Nursing.2024; 36(1): 41. CrossRef - Post-traumatic Growth Experiences of Breast Cancer Survivors: A Grounded Theory Approach
Seung-Kyoung Yang, Young-Suk Park, Eun-Joo Lee
Journal of Korean Association for Qualitative Research.2024; 9(2): 79. CrossRef - Social Reintegration Experiences of Young Adult Cancer Survivors
Ji Seong Yi, Song Yi Lee
Behavioral Sciences.2024; 14(11): 1101. CrossRef - A Structural Equation Model for Posttraumatic Growth among Cured Patients with COVID-19
Soo Young An, Heejung Choi
Journal of Korean Academy of Nursing.2023; 53(3): 309. CrossRef - Effects of Post Traumatic Growth on Successful Aging in Breast Cancer Survivors in South Korea: The Mediating Effect of Resilience and Intolerance of Uncertainty
Su Jeong Yi, Ku Sang Kim, Seunghee Lee, Hyunjung Lee
Healthcare.2023; 11(21): 2843. CrossRef - Pathways to post-traumatic growth in Korean female cancer patients: the mediation effects of coping strategies and resilience
Sumi Choi, Dongil Kim, Ahyoung Cho, Sohyun An, Changhyun Kim, Inhwa Yoo
European Journal of Psychotraumatology.2023;[Epub] CrossRef - Structural Equation Model for Psychosocial Adjustment of Breast Cancer Survivors Based on Family Resilience Model
Jiyoung Seo, Myungsun Yi
Korean Journal of Adult Nursing.2022; 34(2): 178. CrossRef - Cancer coping, healthcare professionals’ support and posttraumatic growth in brain-tumor patients
Jiyoung Kim, Nayeon Shin
Psychology, Health & Medicine.2022; 27(4): 780. CrossRef - Factors Associated with Post-Traumatic Growth in Patients with Breast Cancer Based on a Model of Post-Traumatic Growth
Hee Yeon Park, Ja Yun Choi
Asian Oncology Nursing.2022; 22(2): 65. CrossRef - Factors influencing posttraumatic growth in ovarian cancer survivors
Jeong Min Oh, Yoonjung Kim, Yeunhee Kwak
Supportive Care in Cancer.2021; 29(4): 2037. CrossRef - Factors Influencing Supportive Care Needs of Colorectal Cancer Survivors
Hyekyung Kim, Yang-Sook Yoo
Asian Nursing Research.2021; 15(1): 60. CrossRef - Factors associated with post-traumatic growth in male patients with rectal cancer: A cross-sectional study
Yuri Kim, Yoonjung Kim, Yeunhee Kwak
European Journal of Oncology Nursing.2021; 54: 102028. CrossRef - A Structural Model on the Post-Traumatic Growth of Police Officers
Seung Woo Han, Eun Suk Choi
Journal of Korean Academy of Community Health Nursing.2020; 31(3): 348. CrossRef - Stacking Ensemble Technique for Classifying Breast Cancer
Hyunjin Kwon, Jinhyeok Park, Youngho Lee
Healthcare Informatics Research.2019; 25(4): 283. CrossRef - Factors Influencing Posttraumatic Growth in Cancer Survivors
Jeong-Sook Park, You-Jeong Kim, Young-Seun Ryu, Mi-Hyang Park
Asian Oncology Nursing.2018; 18(1): 30. CrossRef - The relationship between cancer‐related worry and posttraumatic growth in adolescent and young adult cancer survivors
Glynnis A. McDonnell, Alice W. Pope, Tammy A. Schuler, Jennifer S. Ford
Psycho-Oncology.2018; 27(9): 2155. CrossRef - The Influence of Spiritual Well-Being, Self-Esteem, and Perceived Social Support on Post-Traumatic Growth among Breast Cancer Survivors
Eun Young Seo, Suhye Kwon
Asian Oncology Nursing.2018; 18(4): 232. CrossRef
- The influence of locus of control, coping strategies and time perspective on post-traumatic growth in survivors with primary breast cancer
- 1,751 View
- 18 Download
- 20 Crossref

- The Structural Equation Model on Resilience of Breast Cancer Patients Receiving Chemotherapy
- Jeong Ha Yang, Ok Soo Kim
- J Korean Acad Nurs 2016;46(3):327-337. Published online June 30, 2016
- DOI: https://doi.org/10.4040/jkan.2016.46.3.327
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to construct and test a structural equation model on resilience of breast cancer patients receiving chemotherapy.
Methods Participants were 204 patients with breast cancer who received chemotherapy treatment. They participated in a structured interview, which included social support, depression, symptom experience, self-efficacy, hope, resilience, and infection prevention behaviors. Data were analyzed using SPSS/WIN 20.0 and AMOS 18.0.
Results Lower depression (γ=-.33,
p =.020) and symptom experience (γ=-.31,p =.012) and higher self-efficacy (γ=.32,p =.005) and hope (γ=.48,p =.016) were influenced by higher social support. Greater resilience was influenced by lower symptom experience (β=-.18,p =.016), higher self-efficacy (β=.49,p =.023), and higher hope (β=.46,p =.012), and these predictors explained 66.7% of variance in resilience. Greater resilience (β=.54,p =.009) made an impact on greater infection prevention behaviors. Resilience mediated the relations of symptom experience (β=-.10p =.013), self-efficacy (β=.27,p =.006) and hope (β=.25,p =.009) with infection prevention behaviors. These predictors explained 24.9% of variance in infection prevention behaviors.Conclusion The findings of the study suggest that breast cancer patientsw ith greater resilience who are receiving chemotherapy participate in increased infection prevention behaviors. Further research should be conducted to seek intervention strategies that improve breast cancer patients' resilience.
-
Citations
Citations to this article as recorded by- A Structural Equation Model of Resilience in Patients Undergoing Lung Cancer Surgery During the Acute Survival Phase: A Cross-Sectional Study
Miri Kim
Journal of Korean Academy of Fundamentals of Nursing.2025; 32(2): 174. CrossRef - Understanding Intention Triggers in Early Autism Screening Promotion: The Role of Narrative and Framing
Lingfei Wang, Will Grant, Xinyi Jin, Guoyan Wang
Health Communication.2025; : 1. CrossRef - Effects of Telephone-based Self-care Intervention for Gynecologic Cancer Patients Receiving Chemotherapy: A Quasi-Experimental Study
Boyeon Lee, Hyojung Park
Journal of Korean Academy of Fundamentals of Nursing.2023; 30(2): 216. CrossRef - Adaptación a la enfermedad, resiliencia y optimismo en mujeres con cáncer de mama
Marlen Simancas Fernández, Carla Zapata Rueda, Gonzalo Galván Patrignani, Jose Carlos Celedón Rivero, Juan Hernández Padilla
Revista Colombiana de Psiquiatría.2023; 52(4): 280. CrossRef - Adaptation to the disease, resilience and optimism in woman with breast cancer
Marlen Simancas Fernández, Carla Zapata Rueda, Gonzalo Galván Patrignani, Jose Carlos Celedón Rivero, Juan Hernández Padilla
Revista Colombiana de Psiquiatría (English ed.).2023; 52(4): 280. CrossRef - Positive personal resources and psychological distress during the COVID-19 pandemic: resilience, optimism, hope, courage, trait mindfulness, and self-efficacy in breast cancer patients and survivors
Francesca Chiesi, Deborah Vizza, Moira Valente, Rosy Bruno, Chloe Lau, Maria Rosita Campagna, Melania Lo Iacono, Francesco Bruno
Supportive Care in Cancer.2022; 30(8): 7005. CrossRef - A menopausal transition model based on transition theory
Jisoon Kim, Sukhee Ahn
Korean Journal of Women Health Nursing.2022; 28(3): 210. CrossRef - Development and Effect of the Integrated Health Promotion Program for Cancer Survivors Living at Home
Hee Sang Yoon, Eun A Hwang
Journal of Korean Academy of Community Health Nursing.2021; 32(1): 51. CrossRef - Resilience in Patients With Lung Cancer
Jie Zhang, Yizhen Yin, Anni Wang, Hui Li, Juan Li, Silan Yang, Yuchen Wu, Jingping Zhang
Cancer Nursing.2021; 44(6): 465. CrossRef - Mediator Roles of Social Support and Hope in the Relationship Between Body Image Distress and Resilience in Breast Cancer Patients Undergoing Treatment: A Modeling Analysis
Hsin-Tien Hsu, Chiung-Hui Juan, Jyu-Lin Chen, Hsiu-Fen Hsieh
Frontiers in Psychology.2021;[Epub] CrossRef - Structure Equation Modeling for Resilience in Patients with Breast Cancer
Dong Rim Hyun, So Yeun Jun, Chang Wan Jun, Sue Kyung Sohn
Korean Journal of Adult Nursing.2021; 33(2): 87. CrossRef - Factors Influencing Resilience among Korean adolescents and young adult survivors of childhood cancer
Yoon Jung Shin, Eui Geum Oh
European Journal of Oncology Nursing.2021; 53: 101977. CrossRef - Self-efficacy, Hope as Mediators Between Positive Coping and Resilience Among Patients With Gastric Cancer Before the First Chemotherapy
Xiaoting Wu, Haibo Xu, Xiaomin Zhang, Shiyu Han, Liuna Ge, Xiaohui Li, Xinqiong Zhang
Cancer Nursing.2021; 44(1): 79. CrossRef - The relationship between resilience, anxiety and depression among patients with mild symptoms of COVID‐19 in China: A cross‐sectional study
Jie Zhang, Zhen Yang, Xiao Wang, Juan Li, Lili Dong, Fusheng Wang, Yifei Li, Ruihong Wei, Jingping Zhang
Journal of Clinical Nursing.2020; 29(21-22): 4020. CrossRef - Relationship between Self-efficacy and Resilience among Patients with Colorectal Cancer with Stoma: Mediating Effects of Family Support and Medical Staff Support
Mi Na Yun, Kyoung Mi Kim
Korean Journal of Adult Nursing.2020; 32(6): 599. CrossRef - Relationship between cancer stigma, social support, coping strategies and psychosocial adjustment among breast cancer survivors
No Eul Kang, Hye Young Kim, Ji Young Kim, Sung Reul Kim
Journal of Clinical Nursing.2020; 29(21-22): 4368. CrossRef - Resilience and Its Predictors Among Chinese Liver Cancer Patients Undergoing Transarterial Chemoembolization
Caixia Li, Huijuan Lu, Wei Qin, Xiaorong Li, Jingxian Yu, Fang Fang
Cancer Nursing.2019; 42(5): E1. CrossRef - Resilience in Koreans With Cancer
Shin-Young Lee, Haeok Lee, Jacqueline Fawcett, Jeong-Hwan Park
Journal of Hospice & Palliative Nursing.2019; 21(5): 358. CrossRef - Examining spiritual support among African American and Caucasian Alzheimer's caregivers: A risk and resilience study
Scott E. Wilks, Wanda R. Spurlock, Sandra C. Brown, Bettina C. Teegen, Jennifer R. Geiger
Geriatric Nursing.2018; 39(6): 663. CrossRef - Factors Influencing Resilience in Hospitalized Patients with Stroke
Jong Kyung Lee, Ji Yeong Yun
Korean Journal of Adult Nursing.2018; 30(4): 385. CrossRef - Effects of a Group Coaching Program on Depression, Anxiety and Hope in Women with Breast Cancer Undergoing Chemotherapy
So Ryoung Seong, Moon-kyung Cho, Jeeyoon Kim, Yeo Ok Kim
Asian Oncology Nursing.2017; 17(3): 188. CrossRef
- A Structural Equation Model of Resilience in Patients Undergoing Lung Cancer Surgery During the Acute Survival Phase: A Cross-Sectional Study
- 1,757 View
- 23 Download
- 21 Crossref

- Development and Validation of the Empowerment Scale for Woman with Breast Cancer
- Sun Hwa Shin, Hyojung Park
- J Korean Acad Nurs 2015;45(4):613-624. Published online August 31, 2015
- DOI: https://doi.org/10.4040/jkan.2015.45.4.613
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to develop a scale to evaluate empowerment in woman with breast cancer and to examine the validity and reliability of the scale.
Methods The development process for the initial items included a literature review, interviews, and construction of a conceptual framework. The identified items were evaluated for content validity by experts, resulting in 3 factors and 48 preliminary items. Participants were 319 women with breast cancer recruited to test reliability and validity of the preliminary scale. Data were analyzed using item analysis, confirmatory factor analysis, criterion related validity, internal consistency and test-retest reliability.
Results The final scale consisted of 30 items and 3 factors. Factors, including 'intrapersonal factor' (14 items), 'interactional factor' (8 items), and 'behavioral factor' (8 items), were drawn up after confirmatory factor analysis. Goodness of fit of the final research model was very appropriate as shown by χ2/df=1.86, TLI=.90, CFI=.92, SRMR=.06, and RMSEA=.05. Criterion validity was evaluated by total correlation with the Cancer Empowerment Questionnaire .78. Cronbach's alpha for total items was .93 and test-retest reliability was .69.
Conclusion Findings from this study indicate that the scale can be used in the development of nursing interventions to promote the empowerment of women having breast cancer.
-
Citations
Citations to this article as recorded by- Effect of depression and empowerment on medication adherence in patients with breast cancer: a descriptive survey
Sookyung Jeong, Eun Jeong Kim
BMC Nursing.2025;[Epub] CrossRef - Which Chemotherapy-Related Terms Were Difficult for Cancer Patients, and Who Would Have the Most Difficulties?
Mangyeong Lee, Nayeon Kim, Ho-Young Kim, Ayoung Lee, Junghee Yoon, Juhee Cho
Cancer Research and Treatment.2025; 57(3): 669. CrossRef - Empowerment mediates the impact of upper extremity function on posttraumatic growth in breast cancer survivors
Chaewon Yun, Yujin Jeong
Asia-Pacific Journal of Oncology Nursing.2025; 12: 100708. CrossRef - Patient Empowerment in Cancer Care
Soo Hyun Kim, Yu Hyeon Choe, Da Hye Kim
Cancer Nursing.2024; 47(6): 471. CrossRef - Development and Evaluation of Health Empowerment Scale for North Korean Women Defectors
Semi Lim, Younhee Kang
Journal of Korean Academy of Nursing.2022; 52(1): 80. CrossRef - Reliability and Validity of the Korean Version of the Health Care Empowerment Questionnaire (K-HCEQ)
Semi Lim, Kyungmi Lee
Journal of Korean Academy of Fundamentals of Nursing.2022; 29(2): 131. CrossRef - Effects of a partnership‐based, needs‐tailored self‐management support intervention for post‐treatment breast cancer survivors: A randomized controlled trial
Soo Hyun Kim, Yu Hyeon Choe, Young Up Cho, Seho Park, Moon Hee Lee
Psycho-Oncology.2022; 31(3): 460. CrossRef - Concept Analysis of the Empowerment of Patients With Coronary Artery Disease Using a Hybrid Model
Jiyoung Kim, Nayeon Shin
Advances in Nursing Science.2022; 45(1): E31. CrossRef - Application of empowerment education in health education for cancer patients
Yan PENG, Lin HAN, Fang-Fang AN, Li LI, Yue-Li HOU
Journal of Integrative Nursing.2021; 3(1): 46. CrossRef - Development and evaluation of the Coronary Artery Disease Empowerment Scale (CADES) in Korea
Jiyoung Kim, Nayeon Shin, Kyungmi Lee
Clinical Nursing Research.2021; 30(8): 1241. CrossRef - Design of a randomized controlled trial of a partnership-based, needs-tailored self-management support intervention for post-treatment breast cancer survivors
Soo Hyun Kim, Yu Hyeon Choe, Ah Reum Han, Gwui Jeong Yeon, Gyeong Hee Lee, Bo Gyeong Lee, Young Up Cho, Seho Park, Moon Hee Lee
BMC Cancer.2020;[Epub] CrossRef - Reliability and Validity of the Clinical Competency Scale for Nursing Students
Bo Young Kim, Myeong Jeong Chae, Yun Ok Choi
Journal of Korean Academy of Community Health Nursing.2018; 29(2): 220. CrossRef - Development and Validity Testing of an Arthritis Self-Management Assessment Tool
HyunSoo Oh, SunYoung Han, SooHyun Kim, WhaSook Seo
Orthopaedic Nursing.2018; 37(1): 24. CrossRef - Patient empowerment: a systematic review of questionnaires measuring empowerment in cancer patients
Nanna Bjerg Eskildsen, Clara Ruebner Joergensen, Thora Grothe Thomsen, Lone Ross, Susanne Malchau Dietz, Mogens Groenvold, Anna Thit Johnsen
Acta Oncologica.2017; 56(2): 156. CrossRef
- Effect of depression and empowerment on medication adherence in patients with breast cancer: a descriptive survey
- 1,569 View
- 23 Download
- 14 Crossref

- Prevalence and Characteristics of Chemotherapy-related Cognitive Impairment in Patients with Breast Cancer
- Jin-Hee Park, Sun Hyoung Bae, Yong-Sik Jung, Young-Mi Jung
- J Korean Acad Nurs 2015;45(1):118-128. Published online February 27, 2015
- DOI: https://doi.org/10.4040/jkan.2015.45.1.118
-
 Abstract
Abstract
 PDF
PDF Purpose Evidence suggests that some patients with breast cancer experience cognitive difficulties following chemotherapy. This longitudinal study was done to examine the prevalence of cognitive impairment and trajectory of cognitive function over time in women with breast cancer, who received adjuvant chemotherapy.
Methods Participants were 137 patients with breast cancer. They completed neuropsychological tests and the Functional Assessment of Cancer Therapy-Cognitive Function before adjuvant therapy (pretest), toward the end of adjuvant therapy (posttest), and 6 months after the completion of adjuvant therapy (follow-up test). Of the patients, 91 were treated with adjuvant chemotherapy and 46 patients who did not receive chemotherapy made up the comparison group. A reliable-change index and repeated-measure ANOVA were used for statistical analyses.
Results At the posttest point, over 30% of patients showed complex cognitive impairment and reported greater difficulty in subjective cognitive function. At the follow-up test point, 22.0% of patients exhibited complex cognitive impairment and 30.8% of patients complained of subjective cognitive impairment. Repeated-measure ANOVA showed significant decreases after receiving chemotherapy followed by small improvements 6 months after the completion of chemotherapy in cognitive domains of change for attention and concentration, memory, executive function, and subjective cognitive function.
Conclusion These results suggest that chemotherapy in patients with breast cancer may be associated with objective and subjective cognitive impairments. Further studies are needed to explore the potential risk factors and predictor of chemotherapy-related cognitive changes. Also nursing interventions for prevention and intervention of cognitive impairments should be developed and tested.
-
Citations
Citations to this article as recorded by- Impact of nonpharmacological interventions on cognitive impairment in women with breast cancer: A systematic review and meta-analysis
Jin-Hee Park, Su Jin Jung, Lena J. Lee, Junghyun Rhu, Sun Hyoung Bae
Asia-Pacific Journal of Oncology Nursing.2023; 10(4): 100212. CrossRef - Factors Associated with Self-reported Memory Problems of Adult Cancer Survivors Based on the Korea National Health and Nutrition Examination Survey 2019
Sangjin Ko
Journal of Health Informatics and Statistics.2023; 48(1): 51. CrossRef - Brain network deficits in breast cancer patients after early neoadjuvant chemotherapy: A longitudinal MRI study
Jing Yang, Yongchun Deng, Daihong Liu, Yong Tan, Meng Lin, Xiaoyu Zhou, Jing Zhang, Hong Yu, Yixin Hu, Yu Tang, Shixi Jiang, Jiuquan Zhang
Journal of Neuroscience Research.2023; 101(7): 1138. CrossRef - Frailty and its associated factors among older adults with cancer undergoing chemotherapy as outpatients: A cross-sectional study
Misun Jeon, Hyoeun Jang, Arum Lim, Sanghee Kim
European Journal of Oncology Nursing.2022; 60: 102192. CrossRef - The Experience of Chemotherapy Related Cognitive Impairment in Patients with Cancer
Pok Ja Oh, Ji Hyun Kim
Asian Oncology Nursing.2022; 22(1): 1. CrossRef - Distinct sleep disturbance and cognitive dysfunction profiles in oncology outpatients receiving chemotherapy
Vivian Huang, Lynda Mackin, Kord M. Kober, Steven M. Paul, Bruce A. Cooper, Yvette P. Conley, Marilyn J. Hammer, Jon D. Levine, Christine Miaskowski
Supportive Care in Cancer.2022; 30(11): 9243. CrossRef - Measurement, outcomes and interventions of cognitive function after breast cancer treatment: A narrative review
Miaomiao Jia, Xiaojun Zhang, Liyuan Wei, Jinnan Gao
Asia-Pacific Journal of Clinical Oncology.2021; 17(4): 321. CrossRef - Improving preoperative breast reconstruction consultations: a qualitative study on the impact of personalised audio-recordings
Josipa Petric, Bahara Sadri, Phillipa van Essen, Nicola Ruth Dean
BMC Women's Health.2021;[Epub] CrossRef - Study on Neurologic and Cognitive Dysfunction in Breast Cancer Patients Undergoing Chemotherapy with Resting State fMRI
Fenshan Zheng, Peiying Cao, Jie Zhou, Chunyu Li, John Norris
World Neurosurgery.2021; 149: 388. CrossRef - Changes of Cognitive Function and Fatigue following Chemotherapy in Patients with Gastrointestinal Cancer: A Prospective Controlled Study
Pok-Ja Oh, Sun Mi Moon
Asian Oncology Nursing.2019; 19(3): 126. CrossRef - Computerized programs for cancer survivors with cognitive problems: a systematic review
Yoonjung Kim, Sook Jung Kang
Journal of Cancer Survivorship.2019; 13(6): 911. CrossRef - Cancer treatment effects on cognition and depression: The moderating role of physical activity
Margaret F. Bedillion, Emily B. Ansell, Gwendolyn A. Thomas
The Breast.2019; 44: 73. CrossRef - Changes of Cognitive Function and Depression following Chemotherapy in Women with Breast Cancer: A Prospective Study
Pok Ja Oh, Jung Ran Lee, Hyun Ah Kim
Asian Oncology Nursing.2018; 18(2): 66. CrossRef - Mulheres Submetidas à Quimioterapia e suas Funções Cognitivas
Camila Vasconcelos Carnaúba Lima, Raner Miguel Ferreira Póvoa
Psicologia: Ciência e Profissão.2017; 37(4): 970. CrossRef - Chemotherapy-induced prospective memory impairment in breast cancer patients with different hormone receptor expression
Wen Li, Chen Gan, Yue Lv, Shanghu Wang, Huaidong Cheng
Medicine.2017; 96(13): e6514. CrossRef - Altered network efficiency of functional brain networks in patients with breast cancer after chemotherapy
Han Xuan, Chen Gan, Wen Li, Zhonglian Huang, Longsheng Wang, Qianqian Jia, Zhendong Chen, Huaidong Cheng
Oncotarget.2017; 8(62): 105648. CrossRef - Chemotherapy-related Cognitive Impairment and Quality of Life in People with Colon Cancer: The Mediating Effect of Psychological Distress
Pok Ja Oh, Jeong Hye Kim
Journal of Korean Academy of Nursing.2016; 46(1): 19. CrossRef - Effect of Cancer Symptoms and Fatigue on Chemotherapy-related Cognitive Impairment and Depression in People with Gastrointestinal Cancer
Pok Ja Oh, Jung Ran Lee
Journal of Korean Academy of Nursing.2016; 46(3): 420. CrossRef - A review of traditional Korean medical treatment for cancer-related cognitive impairment
Hye-Yoon Lee, Jung-Eun Kim, Mikyung Kim, Joo-Hee Kim
Journal of Korean Medicine.2016; 37(3): 74. CrossRef - Cognitive outcome after radiotherapy in brain tumor
Thomas Durand, Marie-Odile Bernier, Isabelle Léger, Hervé Taillia, Georges Noël, Dimitri Psimaras, Damien Ricard
Current Opinion in Oncology.2015; 27(6): 510. CrossRef - Changes of Symptom Distress and Quality of Life in Breast Cancer Patients Receiving Adjuvant Therapy
Jin-Hee Park, Sun Hyoung Bae, Young-Mi Jung
Asian Oncology Nursing.2015; 15(2): 67. CrossRef
- Impact of nonpharmacological interventions on cognitive impairment in women with breast cancer: A systematic review and meta-analysis
- 1,621 View
- 19 Download
- 21 Crossref

- Factors Influencing Quality of Life in Patients with Breast Cancer on Hormone Therapy
- Eunkyung Hwang, Myungsun Yi
- J Korean Acad Nurs 2014;44(1):108-117. Published online February 28, 2014
- DOI: https://doi.org/10.4040/jkan.2014.44.1.108
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of the study was to identify degrees of pain, menopause symptoms, and quality of life, and to identify factors influencing quality of life of patients with breast cancer who were on hormone therapy.
Methods A cross-sectional survey design was utilized. Data were collected using questionnaires from 110 patients with breast cancer who had been on hormone therapy for 3 months or more and were being treated at a university hospital in Seoul. Data were analyzed using χ2-test, t-test, ANOVA, Pearson correlation coefficient and multiple linear regression.
Results Mean age of the participants was 53.56 (SD=6.67) and 54 (51.4%) had stage 0 or I at the time of diagnosis. Most of the participants reported having pain and menopause symptoms (88.2% and 95.5% respectively). The mean score for quality of life was 87.84±21.17. Pain, menopause symptoms and quality of life had strong correlations with each other (
p <.005). Quality of life was explained by menopause symptoms (β= -.71), economic status (β=.20) and occupation (β=.16).Conclusion The results of the study suggest that menopause symptoms should be incorporated into oncologic nursing care to improve quality of life of patients with breast cancer on hormone therapy.
-
Citations
Citations to this article as recorded by- Factors Associated With Quality of Life Among Posttreatment Cancer Survivors in Korea
Soo Hyun Kim, Yu Hyeon Choe, Jingyeong Choi, Ji Young Park, Eun Yi
Cancer Nursing.2025; 48(1): E47. CrossRef - Effects of Functional Glide on lymphedema, Handgrip strength, and Quality of Life in Patients with Breast Cancer
Hyunah Lee, Dongkwon Seo
Physical Therapy Rehabilitation Science.2024; 13(4): 524. CrossRef - Traditional Korean Medicine Treatment for Sequelae After Tamoxifen in Breast Cancer Patients: Two Case Reports
Jung-min Yang, Jae-woo Yang, Ji-hoon Oh, Woo-seok Hwang
The Journal of Internal Korean Medicine.2023; 44(1): 53. CrossRef - Impacts of Uncertainty and Social Support on the Quality of Life of Breast Cancer Survivors after Chemotherapy: Based on Self-help Group Participants
Hyenam Hwang, Yoonshin Lee
Asian Oncology Nursing.2023; 23(4): 177. CrossRef - Factors associated with the quality of work life among working breast cancer survivors
Juhyun Jin
Asia-Pacific Journal of Oncology Nursing.2022; 9(2): 97. CrossRef - Perceived New Normal and Inner Strength on Quality of Life in Breast Cancer Patients Receiving Adjuvant Endocrine Therapy
Sujin Ha, Eunjung Ryu
Asia-Pacific Journal of Oncology Nursing.2021; 8(4): 377. CrossRef - Unmet Needs and Quality of Life of Cancer Patients and Their Families: Actor–Partner Interdependence Modeling
Yubeen Jang, Younhee Jeong
Healthcare.2021; 9(7): 874. CrossRef - Photovoice-Based Assessment of Weight Management Experiences of Breast Cancer Patients Treated with Tamoxifen
Jung Suk Park, Jeong-Won Han, Jin Hyuk Choi, Kyoung Chun Lee
International Journal of Environmental Research and Public Health.2020; 17(12): 4359. CrossRef - Effects of Illness Perception and Health Beliefs on the Quality of Life of Breast Cancer Patients in the Yanbian Area of China
Fenshan Zheng, Ogcheol Lee, Jie Zhou, Chunyu Li
Asian Oncology Nursing.2019; 19(3): 135. CrossRef - Effects of Menopausal Symptoms and Depression on the Quality of Life of Premenopausal Women With Breast Cancer in Korea
Jeong Ae Han, So Young Choi, Seonah Lee
Journal of Transcultural Nursing.2019; 30(1): 8. CrossRef - Pain and Menopause Symptoms of Breast Cancer Patients with Adjuvant Hormonal Therapy in Korea: Secondary Analysis
Myungsun Yi, Eunkyung Hwang
Asia-Pacific Journal of Oncology Nursing.2018; 5(3): 262. CrossRef - Predictors of the quality of life in Chinese breast cancer survivors
Juan Xia, Zheng Tang, Qinglong Deng, Renren Yang, Jiwei Wang, Jinming Yu
Breast Cancer Research and Treatment.2018; 167(2): 537. CrossRef - How Menopause Symptoms and Attitude Impact Korean Women's Quality of Life After Adjuvant Treatment for Breast Cancer
Moonhee Gang, Mi Sook Jung, Sunyoung Park, Younghee Park, Kyongok Oh
Cancer Nursing.2017; 40(6): E60. CrossRef - Validity and Reliability of the Korean Version of the Beliefs about Medicines Questionnaire-Specific for Breast Cancer Patients on Hormone Therapy
Younglan Kim, Yul Ha Min
Journal of Health Informatics and Statistics.2017; 42(2): 136. CrossRef - Effect of Abdominal Skin Massage and Warming Therapy on the Pain and Anxiety in Breast Cancer Patients who Underwent Hormone Injections
Jin Hee Jun, Youn Ok Lee, Se-Na Lee
Asian Oncology Nursing.2016; 16(4): 226. CrossRef - Psychometric Properties of the Korean Version of the Inner Strength Questionnaire
Suhyeon Choi, Eunjung Ryu
Asian Oncology Nursing.2016; 16(1): 38. CrossRef - Changes of Supportive Care Needs and Quality of Life in Patients with Breast Cancer
Jin-Hee Park, Mison Chun, Yong-Sik Jung, Young-Mi Jung
Asian Oncology Nursing.2016; 16(4): 217. CrossRef - Effects of Trogopterorum Faeces on the Apoptostic Cell Death in Breast Cancer Cells
Yu-Rim Song, Ji-Eun Kim, Seung-Jeong Yang, Kyung-Mi Park, Su-Jung Jung, Seong-Hee Cho
The Journal of Oriental Obstetrics and Gynecology.2015; 28(1): 46. CrossRef - Fatigue, Sleep Disturbance, and Quality of Life among Breast Cancer Patients Receiving Radiotherapy
Ran Young Kim, Hyojung Park
Korean Journal of Adult Nursing.2015; 27(2): 188. CrossRef
- Factors Associated With Quality of Life Among Posttreatment Cancer Survivors in Korea
- 1,401 View
- 3 Download
- 19 Crossref

- Posttraumatic Growth of Patients with Breast Cancer
- Sook Lee, Yeon Jung Kim
- J Korean Acad Nurs 2012;42(6):907-915. Published online December 31, 2012
- DOI: https://doi.org/10.4040/jkan.2012.42.6.907
-
 Abstract
Abstract
 PDF
PDF Purpose A diagnosis of breast cancer is one of the most traumatic events that threatens a woman's life, but while women adapt to and overcome these threats, they not only experience negative aspects, but also growth. The purpose of this study was to identify the many factors that affect growth, and to provide fundamental information for nursing interventions, which can help the women in their growth.
Methods The participants in this study were 131 married women patients with breast cancer, who were on medical treatment in one of two university hospitals, in Seoul and Chungnam. Data were collected for posttraumatic growth, self-esteem, cancer coping questionnaire, marital intimacy, and body image. The data were analyzed using the SPSS 19.0 program (IBM).
Results Interpersonal cancer coping, intrapersonal cancer coping (planning) and self-esteem accounted for 29.0% of posttraumatic growth.
Conclusion These findings indicate that in order to help the women's growth after the trauma of breast cancer, it is necessary to enhance their self-esteem, and to develop psycho-social nursing supportive programs.
-
Citations
Citations to this article as recorded by- Structural Equation Model for Psychosocial Adjustment of Breast Cancer Survivors Based on Family Resilience Model
Jiyoung Seo, Myungsun Yi
Korean Journal of Adult Nursing.2022; 34(2): 178. CrossRef - Development and effects of a post-traumatic growth program for patients with breast cancer
Sung Hee Choi, Young Whee Lee, Hwa Soon Kim, Soo Hyun Kim, Eun-Hyun Lee, Eun Young Park, Young Up Cho
European Journal of Oncology Nursing.2022; 57: 102100. CrossRef - Posttraumatic Growth and Health Promotion Behavior in Patients with Cancer: The Mediating Effect of Spiritual Well-Being
Shunji Piao, Pok Ja Oh
Asian Oncology Nursing.2021; 21(1): 33. CrossRef - The effectiveness of acceptance and commitment therapy on the rate of acceptance and post-traumatic growth in colorectal cancer patients comorbid with stress
Ahmad kazemipour, Fazlolah mirderikvand, Kourosh amraei
Health Monitor Journal of the Iranian Institute for Health Sciences Research.2020; 19(5): 569. CrossRef - Post-traumatic Growth among Stroke Patients: Impact of Hope, Meaning in Life, and Social Support
Young-Ju Jeong, Hee Sun Kim
Korean Journal of Adult Nursing.2019; 31(6): 605. CrossRef - A Structural Equation Model of Factors Influencing Posttraumatic Growth of Earthquake Victims
Minyeong Kwak
Journal of Korean Academy of Community Health Nursing.2019; 30(3): 345. CrossRef - Factors Influencing Posttraumatic Growth of Gynecologic Oncology Patients Undergoing Chemotherapy
Sun Jeong Yun, Hye Young Kim
Korean Journal of Women Health Nursing.2019; 25(4): 409. CrossRef - The Influence of Spiritual Well-Being, Self-Esteem, and Perceived Social Support on Post-Traumatic Growth among Breast Cancer Survivors
Eun Young Seo, Suhye Kwon
Asian Oncology Nursing.2018; 18(4): 232. CrossRef - The Relationship between Post-Traumatic Growth, Trauma Experience and Cognitive Emotion Regulation in Nurses
Sook Lee, Mun Gyeong Gwon, YeonJung Kim
Korean Journal of Stress Research.2018; 26(1): 31. CrossRef - Posttraumatic growth in breast cancer survivors and their husbands based on the actor‐partner interdependence model
MyoSuk Lee, Kyunghee Kim, Changwon Lim, Ji‐Su Kim
Psycho-Oncology.2017; 26(10): 1586. CrossRef - Comparison of Perception of Successful Aging between Late Middle-aged Breast Cancer Survivors and Healthy Women
Eun Ja Kim, Nahyun Kim
Journal of Korean Gerontological Nursing.2017; 19(1): 48. CrossRef - Self-Efficacy, Self-Care Behavior, Posttraumatic Growth, and Quality of Life in Patients with Cancer according to Disease Characteristics
Jinho Choi, Sunyoung Lee, Byungduck An
The Korean Journal of Hospice and Palliative Care.2016; 19(2): 170. CrossRef - The Effects of Self-esteem and Problem Focused Coping on Post-traumatic Growth among Police Officers
Seung Woo Han, Eunsuk Choi
Korean Journal of Occupational Health Nursing.2016; 25(3): 141. CrossRef - Factors Influencing Posttraumatic Growth in Survivors of Breast Cancer
Jin-Hee Park, Yong-Sik Jung, Youngmi Jung
Journal of Korean Academy of Nursing.2016; 46(3): 454. CrossRef - Factors Related to Posttraumatic Growth in Patients with Colorectal Cancer
Hyeon Ju Lee, Seong Sook Jun
Korean Journal of Adult Nursing.2016; 28(3): 247. CrossRef - Influencing Factors for Post-traumatic Growth in Patients with Breast Cancer
Sung-Hee Choi, Young-Whee Lee
The Journal of the Korea Contents Association.2016; 16(11): 499. CrossRef - The Effects of Posttraumatic Growth and Meaning in Life on Health Promotion Behavior in Cancer Patients
Sun-Hee Jang, Hae-Rang Lee, Hyung-Nam Yeu, Soon-Ock Choi
Asian Oncology Nursing.2014; 14(2): 100. CrossRef - Posttraumatic Growth, Dyadic Adjustment, and Quality of Life in Breast Cancer Survivors and Their Husbands
Seunghee Song, Eunjung Ryu
Journal of Korean Academy of Nursing.2014; 44(5): 515. CrossRef - Changes of Self-efficacy, Depression, and Posttraumatic Growth in Survivors with Breast Cancer Participating Breast Cancer Prevention Volunteering
Myungsun Yi, Jieun Cha, Youngmi Ryu
The Journal of the Korea Contents Association.2014; 14(4): 256. CrossRef - Effects of a Cancer-Overcome BeHaS Exercise Program on Post-trauma Risk and Anxiety in Breast Cancer Patients
Sun Ae Kim, Jong Im Kim, Sun Young Park
Journal of muscle and joint health.2014; 21(1): 27. CrossRef
- Structural Equation Model for Psychosocial Adjustment of Breast Cancer Survivors Based on Family Resilience Model
- 1,223 View
- 10 Download
- 20 Crossref

- A Meta-analysis of Chemotherapy related Cognitive Impairment in Patients with Breast Cancer
- Jin-Hee Park, Sun Hyoung Bae
- J Korean Acad Nurs 2012;42(5):644-658. Published online October 12, 2012
- DOI: https://doi.org/10.4040/jkan.2012.42.5.644
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to evaluate the cognitive effects of chemotherapy in patients with breast cancer.
Methods Using several databases, prospective studies were collected up to August 2011. Of 2,106 publications identified, 12 met the inclusion criteria, and 8 studies were used to estimate the effect size of chemotherapy on cognitive impairment.
Results Twelve studies were done since 2005 and most of the research was performed in Europe or North America. Eight studies were used to generate effect size across the cognitive domains of attention/concentration, verbal and visual memory, executive function, visuospatial skill, language, and subjective cognitive function. Each of the cognitive domains showed small effect sizes (-0.02 ~ -0.26), indicating diminished cognitive function for the chemotherapy group compared with non-chemotherapy groups.
Conclusion Finding suggests that breast cancer patients who undergo chemotherapy may experience mild cognitive decline. Further study is needed to generate knowledge and guideline for interventions to address chemotherapy related cognitive impairment in these patients.
-
Citations
Citations to this article as recorded by- The Experience of Chemotherapy Related Cognitive Impairment in Patients with Cancer
Pok Ja Oh, Ji Hyun Kim
Asian Oncology Nursing.2022; 22(1): 1. CrossRef - Effects of smart-care services program for breast cancer survivors
Bok Yae Chung, Sung Jung Hong
The Journal of Korean Academic Society of Nursing Education.2021; 27(2): 95. CrossRef - Changes of Cognitive Function and Fatigue following Chemotherapy in Patients with Gastrointestinal Cancer: A Prospective Controlled Study
Pok-Ja Oh, Sun Mi Moon
Asian Oncology Nursing.2019; 19(3): 126. CrossRef - Effects of compensatory cognitive training intervention for breast cancer patients undergoing chemotherapy: a pilot study
Jin-Hee Park, Yong Sik Jung, Ku Sang Kim, Sun Hyoung Bae
Supportive Care in Cancer.2017; 25(6): 1887. CrossRef - Impact of Cognitive Function and Cancer Coping on Quality of Life among Women with Post-chemotherapy Breast Cancer
Yoon Jung Kim, Sook Jung Kang
Korean Journal of Women Health Nursing.2016; 22(3): 182. CrossRef - Chemotherapy-related Cognitive Impairment and Quality of Life in People with Colon Cancer: The Mediating Effect of Psychological Distress
Pok Ja Oh, Jeong Hye Kim
Journal of Korean Academy of Nursing.2016; 46(1): 19. CrossRef - QLU-C10D: a health state classification system for a multi-attribute utility measure based on the EORTC QLQ-C30
M. T. King, D. S. J. Costa, N. K. Aaronson, J. E. Brazier, D. F. Cella, P. M. Fayers, P. Grimison, M. Janda, G. Kemmler, R. Norman, A. S. Pickard, D. Rowen, G. Velikova, T. A. Young, R. Viney
Quality of Life Research.2016; 25(3): 625. CrossRef - The Impact of Cancer on Psychological and Social Outcomes
Daniel Sj Costa, Rebecca Mercieca‐bebber, Claudia Rutherford, Liam Gabb, Madeleine T King
Australian Psychologist.2016; 51(2): 89. CrossRef - Prevalence and Characteristics of Chemotherapy-related Cognitive Impairment in Patients with Breast Cancer
Jin-Hee Park, Sun Hyoung Bae, Yong-Sik Jung, Young-Mi Jung
Journal of Korean Academy of Nursing.2015; 45(1): 118. CrossRef
- The Experience of Chemotherapy Related Cognitive Impairment in Patients with Cancer
- 1,370 View
- 5 Download
- 9 Crossref

- Development and Effectiveness of Expressive Writing Program for Women with Breast Cancer in Korea
- Eun Young Park, Mungsun Yi
- J Korean Acad Nurs 2012;42(2):269-279. Published online April 30, 2012
- DOI: https://doi.org/10.4040/jkan.2012.42.2.269
-
 Abstract
Abstract
 PDF
PDF Purpose To develop a expressive writing program for women with breast cancer and to identify its effects on stress physical symptom, cancer symptom, anxiety, depression, and QOL.
Methods A non-equivalent control pre-post design was used. Participants were recruited from self-help groups in six hospitals and were assigned to the experimental group (29) or control group (29). Data were collected before, after, and at four weeks after the intervention program. Changes in the variables were evaluated to test effects of the developed program, using χ2-test, Fisher's exact test, repeated measures ANOVA, and paired t-test.
Results The expressive writing program was developed for women with breast cancer based on Pennebaker's expressive writing. Significant differences were found between the two groups for stress related to physical symptoms (
p <.00) and quality of life (p =.024). No significant differences were found in cancer symptoms, anxiety, or depression between the two groups.Conclusion The results indicate that the expressive writing program designed to express cancer-related deep thoughts and emotions helps in decreasing physical symptoms and improving QOL. Further studies are needed to identify the effect on emotions such as anxiety and depression for women with breast cancer with above average levels of anxiety and depression.
-
Citations
Citations to this article as recorded by- Effects of a Remote Videoconferencing-based Expressive Writing Program on Posttraumatic Stress, Resilience, and Post-traumatic Growth among Traumatized Nurses
Nam Hee Chae, Ji Young Kim
Journal of Korean Academy of Nursing Administration.2024; 30(2): 152. CrossRef - Care Needs of Advanced Cancer Patients in a Long-term Care Hospital: Patient-Nurse Comparison
Hee-Jung Kang, Kyung-Ah Kang
Asian Oncology Nursing.2023; 23(4): 196. CrossRef - Can emotional expressivity and writing content predict beneficial effects of expressive writing among breast cancer patients receiving chemotherapy? A secondary analysis of randomized controlled trial data from China
Yanni Wu, Dongliang Yang, Biao Jian, Chaixiu Li, Liping Liu, Wenji Li, Xiaojin Li, Chunlan Zhou
Psychological Medicine.2023; 53(4): 1527. CrossRef - Development and effects of a post-traumatic growth program for patients with breast cancer
Sung Hee Choi, Young Whee Lee, Hwa Soon Kim, Soo Hyun Kim, Eun-Hyun Lee, Eun Young Park, Young Up Cho
European Journal of Oncology Nursing.2022; 57: 102100. CrossRef - Effect of Expressive Writing on Professional Quality of Life and Resilience among Intensive Care Unit Nurses
Danbi You, Hye-Ja Park
Journal of Health Informatics and Statistics.2021; 46(3): 276. CrossRef - Effect of prolonged expressive writing on health outcomes in breast cancer patients receiving chemotherapy: a multicenter randomized controlled trial
Yanni Wu, Liping Liu, Wanting Zheng, Chunrao Zheng, Min Xu, Xiaohong Chen, Wenji Li, Lijun Xie, Pengyan Zhang, Xiaoli Zhu, Chuanglian Zhan, Chunlan Zhou
Supportive Care in Cancer.2021; 29(2): 1091. CrossRef - Non-pharmacological therapies for depressive symptoms in breast cancer patients: Systematic review and meta-analysis of randomized clinical trials
Liliana Coutiño-Escamilla, Maricela Piña-Pozas, Aurelio Tobías Garces, Brenda Gamboa-Loira, Lizbeth López-Carrillo
The Breast.2019; 44: 135. CrossRef - The Effects of Expressive Writing Interventions for Patients With Cancer: A Meta-Analysis
Pok-Ja Oh, Soo Kim
Oncology Nursing Forum.2016; 43(4): 468. CrossRef - Does therapeutic writing help people with long-term conditions? Systematic review, realist synthesis and economic considerations
Olga P Nyssen, Stephanie JC Taylor, Geoff Wong, Elizabeth Steed, Liam Bourke, Joanne Lord, Carol A Ross, Sheila Hayman, Victoria Field, Ailish Higgins, Trisha Greenhalgh, Catherine Meads
Health Technology Assessment.2016; 20(27): 1. CrossRef - Effect of Expressive Writing Intervention on Health Outcomes in Breast Cancer Patients: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
Chunlan Zhou, Yanni Wu, Shengli An, Xiaojin Li, Gozde Ozakinci
PLOS ONE.2015; 10(7): e0131802. CrossRef - Expressive writing interventions in cancer patients: a systematic review
Erin L. Merz, Rina S. Fox, Vanessa L. Malcarne
Health Psychology Review.2014; 8(3): 339. CrossRef - Factors Affecting Symptom Experiences of Breast Cancer Patients: Based on the Theory of Unpleasant Symptoms
HyoJin Kim, Sanghee Kim, Hyangkyu Lee, SangEun Oh
Asian Oncology Nursing.2014; 14(1): 7. CrossRef - Written emotional disclosure for women with ovarian cancer and their partners: randomised controlled trial
Emily Arden‐Close, Yori Gidron, Louise Bayne, Rona Moss‐Morris
Psycho-Oncology.2013; 22(10): 2262. CrossRef - Effect of Depression and Anxiety on Symptoms in Thyroid Cancer Patients Undergoing Radioactive Iodine (I131) Therapy
Nami Chun
Asian Oncology Nursing.2012; 12(4): 297. CrossRef - The Relationships between Stigma, Distress, and Quality of Life in Patients with Lung Cancer
Jung Lim Lee, Keum Soon Kim
Journal of Korean Oncology Nursing.2011; 11(3): 237. CrossRef
- Effects of a Remote Videoconferencing-based Expressive Writing Program on Posttraumatic Stress, Resilience, and Post-traumatic Growth among Traumatized Nurses
- 2,055 View
- 18 Download
- 15 Crossref

- Development and Evaluation of 「Hospice Smart Patient」 Service Program
- Chai-Soon Park, Yang-Sook Yoo, Dong-Won Choi, Hyun-Jeong Park, Ji-In Kim
- J Korean Acad Nurs 2011;41(1):9-17. Published online February 28, 2011
- DOI: https://doi.org/10.4040/jkan.2011.41.1.9
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to develop and implement the Hospice Smart Patient Program and to evaluate its effectiveness.
Methods It was quasi-experimental non-equivalent pre-post study. Breast cancer patients who underwent surgery, chemotherapy or radiotherapy, or who needed palliative care, participated in the study. Participants were divided into two groups, experimental and control groups based on their preferences. The program was developed after literature review and discussion among experts on hospice and palliative care. Participants who were in the experimental group received either face-to-face or phone 「Hospice Smart Patient」 Service at least once a week for 5 months.
Results There was a significant difference in quality of life and communication skill between the two groups after the service was provided. In addition, participants in experimental group showed improved decision making skills, mastery sense, and understanding of hospice and palliative care, which would be beneficial in improving their quality of life.
Conclusion We have concluded that the 「Hospice Smart Patient」 Program is useful for cancer patients in decision making, improving self-control and choosing hospice care to improve their quality of life.
-
Citations
Citations to this article as recorded by- Palliative care in the treatment of women with breast cancer: A scoping review
Romel Jonathan Velasco Yanez, Ana Fátima Carvalho Fernandes, Erilaine de Freitas Corpes, Régia Christina Moura Barbosa Castro, Judith Sixsmith, Luís Carlos Lopes-Júnior
Palliative and Supportive Care.2024; 22(3): 592. CrossRef - Efficacy of a Digital Health Tool on Contraceptive Ideation and Use in Nigeria: Results of a Cluster-Randomized Control Trial
Stella Babalola, Caitlin Loehr, Olamide Oyenubi, Akinsewa Akiode, Allison Mobley
Global Health: Science and Practice.2019; 7(2): 273. CrossRef - Psychometric Properties of the Korean Version of the HIV Self-Management Scale in Patients with HIV
Gwang Suk Kim, Sang Hui Chu, Yunhee Park, Jun Yong Choi, Jeong In Lee, Chang Gi Park, Linda L. McCreary
Journal of Korean Academy of Nursing.2015; 45(3): 439. CrossRef - Effectiveness and cost-effectiveness of home palliative care services for adults with advanced illness and their caregivers
Barbara Gomes, Natalia Calanzani, Vito Curiale, Paul McCrone, Irene J Higginson, Maja de Brito
Cochrane Database of Systematic Reviews.2013;[Epub] CrossRef
- Palliative care in the treatment of women with breast cancer: A scoping review
- 1,335 View
- 2 Download
- 4 Crossref

- Symptom Experience and Quality of Life in Breast Cancer Survivors
- Jin Hee Park, Eun-Young Jun, Mi-Young Kang, Yong-Sik Joung, Gu-Sang Kim
- J Korean Acad Nurs 2009;39(5):613-621. Published online October 31, 2009
- DOI: https://doi.org/10.4040/jkan.2009.39.5.613
-
 Abstract
Abstract
 PDF
PDF Purpose The purposes of this study were to evaluate symptom experience and quality of life (QOL) and to identify the predictors of QOL among breast cancer survivors.
Methods A cross-sectional study was conducted on 200 disease-free breast cancer survivors at two hospitals between December 2007 and July 2008. Functional Assessment of Cancer Therapy Scale-B, Memorial Symptom Assessment Scale-short Form and The Linear Analogue Self Assessment Scale were used to assess symptom experience and QOL in these patients. Data were analyzed using the Pearson correlation, t-test, ANOVA, and stepwise multiple regression with SPSS/WIN 12.0.
Results The mean score of QOL for breast cancer survivors was 95.81 (±18.02). The highest scores among physical and psychological symptoms were sexual interest and anxiety. Year since treatment completion was significantly associated with QOL in sociodemographic variables. Physical and psychological symptoms have a significant negative association with QOL. The results of the regression analyses showed that physical and psychological symptoms were statistically significant in predicting patients' QOL.
Conclusion Symptom experience and QOL are essential variables that should be acknowledged when delivering health care to breast cancer survivors. More attention to the reduction and management of psychological distress could improve QOL among breast cancer survivors.
-
Citations
Citations to this article as recorded by- Prediction Model for Postoperative Quality of Life Among Breast Cancer Survivors Along the Survivorship Trajectory From Pretreatment to 5 Years: Machine Learning–Based Analysis
Danbee Kang, Hyunsoo Kim, Juhee Cho, Zero Kim, Myungjin Chung, Jeong Eon Lee, Seok Jin Nam, Seok Won Kim, Jonghan Yu, Byung Joo Chae, Jai Min Ryu, Se Kyung Lee
JMIR Public Health and Surveillance.2023; 9: e45212. CrossRef - Impact of post-treatment symptoms on supportive care needs among breast cancer survivors in South Korea
Unhee Kim, Ju-Young Lee
Asia-Pacific Journal of Oncology Nursing.2023; 10(10): 100295. CrossRef - The Influence of Anxiety, Uncertainty, and Cancer Coping on the Quality of Life in Breast Cancer Patients Receiving Neoadjuvant Chemotherapy
Dong-Rim Hyun, Young Suk Kim
Asian Oncology Nursing.2022; 22(1): 37. CrossRef - Association between sleep quality, anxiety and depression among Korean breast cancer survivors
Ok‐Hee Cho, Kyung‐Hye Hwang
Nursing Open.2021; 8(3): 1030. CrossRef - Determinants of quality of life in women immediately following the completion of primary treatment of breast cancer: A cross-sectional study
Jin-Hee Park, Yong Sik Jung, Ji Young Kim, Sun Hyoung Bae, Ka Ming Chow
PLOS ONE.2021; 16(10): e0258447. CrossRef - Unmet Needs for Job Maintenance of Breast Cancer Survivors
Su Jeong Han, Hye Won Kim, Mi Ran Kim
Journal of Korean Academy of Fundamentals of Nursing.2020; 27(3): 298. CrossRef - Analysis of Health management Awareness and Practice Experience of Breast Cancer Survivors using Focus Group Interviews
Hye Won Kim, Su Jeong Han, Mi Ran Kim
The Korean Journal of Rehabilitation Nursing.2020; 23(1): 48. CrossRef - Effects of Self-Lymph Massage Method among Breast Cancer Survivors
Hyenam Hwang
The Korean Journal of Rehabilitation Nursing.2020; 23(2): 112. CrossRef - The mediating effect of social support on uncertainty in illness and quality of life of female cancer survivors: a cross-sectional study
Insook Lee, Changseung Park
Health and Quality of Life Outcomes.2020;[Epub] CrossRef - Exercise Program Based on Preferences of Breast Cancer Survivors
Ji Yong Byeon, Min Jae Kang, Ji Hye Park, Ji Hee Min, Justin Y. Jeon
The Korean Journal of Physical Education.2018; 57(2): 611. CrossRef - Effects of Auricular Acupressure on Constipation in Patients With Breast Cancer Receiving Chemotherapy: A Randomized Control Trial
Jeongran Shin, Hyojung Park
Western Journal of Nursing Research.2018; 40(1): 67. CrossRef - Factors influencing the quality of life of patients with advanced cancer
Sun-A Park, Seung Hyun Chung, Youngjin Lee
Applied Nursing Research.2017; 33: 108. CrossRef - Effects of a Group Coaching Program on Depression, Anxiety and Hope in Women with Breast Cancer Undergoing Chemotherapy
So Ryoung Seong, Moon-kyung Cho, Jeeyoon Kim, Yeo Ok Kim
Asian Oncology Nursing.2017; 17(3): 188. CrossRef - The Influences of Quality of Sleep and Mood State on Fatigue in Primary Brain Tumor Patients
Jae Hyun Hwang, Hyoung Sook Park
Asian Oncology Nursing.2017; 17(2): 87. CrossRef - Chemotherapy-related Cognitive Impairment and Quality of Life in People with Colon Cancer: The Mediating Effect of Psychological Distress
Pok Ja Oh, Jeong Hye Kim
Journal of Korean Academy of Nursing.2016; 46(1): 19. CrossRef - Effects of a self-managed home-based walking intervention on psychosocial health outcomes for breast cancer patients receiving chemotherapy: a randomised controlled trial
Kajal Gokal, Deborah Wallis, Samreen Ahmed, Ion Boiangiu, Kiran Kancherla, Fehmidah Munir
Supportive Care in Cancer.2016; 24(3): 1139. CrossRef - Return-to-Work Experiences among Nurses after Receiving Cancer Treatment
Mi-Hye Kim, Jeong-Seon Kim, Han-Na Kim
Journal of the Korea Academia-Industrial cooperation Society.2016; 17(6): 215. CrossRef - Development and Validation of the Empowerment Scale for Woman with Breast Cancer
Sun Hwa Shin, Hyojung Park
Journal of Korean Academy of Nursing.2015; 45(4): 613. CrossRef - Changes of Symptom Distress and Quality of Life in Breast Cancer Patients Receiving Adjuvant Therapy
Jin-Hee Park, Sun Hyoung Bae, Young-Mi Jung
Asian Oncology Nursing.2015; 15(2): 67. CrossRef - Validity and reliability of EQ-5D-3L for breast cancer patients in Korea
Seon-Ha Kim, Min-Woo Jo, Jong-Won Lee, Hyeon-Jeong Lee, Jong Kyung Kim
Health and Quality of Life Outcomes.2015;[Epub] CrossRef - Factors that Influence Korean Breast Cancer Patients to Undergo Cancer Rehabilitation Therapy
Hui-jeong Park, Kyunghee Kim, Ji-su Kim
Asian Oncology Nursing.2015; 15(2): 106. CrossRef - Changes of Self-efficacy, Depression, and Posttraumatic Growth in Survivors with Breast Cancer Participating Breast Cancer Prevention Volunteering
Myungsun Yi, Jieun Cha, Youngmi Ryu
The Journal of the Korea Contents Association.2014; 14(4): 256. CrossRef - Body Image and Physical suffering during Radiotherapy in Breast Cancer Patients Following Breast Conserving Operations
Mi Ok Han, Jeong Yun Park
Asian Oncology Nursing.2014; 14(3): 155. CrossRef - Effect of brief psychoeducation using a tablet PC on distress and quality of life in cancer patients undergoing chemotherapy: a pilot study
Joo-Young Lee, Hye Yoon Park, Dooyoung Jung, Mihye Moon, Bhumsuk Keam, Bong-Jin Hahm
Psycho-Oncology.2014; 23(8): 928. CrossRef - Factors Influencing Quality of Life in Patients with Breast Cancer on Hormone Therapy
Eunkyung Hwang, Myungsun Yi
Journal of Korean Academy of Nursing.2014; 44(1): 108. CrossRef - Effects of Resilience, Post-traumatic Stress Disorder on the Quality of Life in Patients with Breast Cancer
Boo Young Ha, Eun Jung Jung, So Young Choi
Korean Journal of Women Health Nursing.2014; 20(1): 83. CrossRef - Menopausal symptoms, sexual function, depression, and quality of life in Korean patients with breast cancer receiving chemotherapy
Hyojung Park, Hyeon Gyeong Yoon
Supportive Care in Cancer.2013; 21(9): 2499. CrossRef - Anxiety, Depression and Uncertainty in Cancer Patients Participating in Clinical Trial of Anticancer Drugs
Haejin Kim, Myungsun Yi
Korean Journal of Adult Nursing.2013; 25(1): 53. CrossRef - Factors Influencing on Quality of Life in Gynecological Cancer Patients
Jeong-Sook Park, Yun-Jung Oh
Korean Journal of Adult Nursing.2012; 24(1): 52. CrossRef - Impacts of Fatigue, Pain, Anxiety, and Depression on the Quality of Life in Patients with Breast Cancer
Hye Sun Byun, Gyung Duck Kim
Asian Oncology Nursing.2012; 12(1): 27. CrossRef - A comparison of quality of life and satisfaction of women with early-stage breast cancer treated with breast conserving therapy vs. mastectomy in southern China
Z.-Y. He, Q. Tong, S.-G. Wu, F.-Y. Li, H.-X. Lin, X.-X. Guan
Supportive Care in Cancer.2012; 20(10): 2441. CrossRef - Quality of Life and Symptom Experience in Breast Cancer Survivors After Participating in a Psychoeducational Support Program
Jin-Hee Park, Sun Hyoung Bae, Yong Sik Jung, Ku Sang Kim
Cancer Nursing.2012; 35(1): E34. CrossRef - Effects of Symptom Severity and Symptom Interference on Sleep Disturbance in Cancer Patients
Kyunghee Kim, Da Hye Park, Darlee Park, Eunjung Ryu
Asian Oncology Nursing.2012; 12(4): 339. CrossRef - Factors affecting the quality of life of middle‐aged women suffering Hwa‐Byung
Young Mi Lim, In Chul Jung, Bok Nam Seo
Journal of Clinical Nursing.2012; 21(15-16): 2377. CrossRef - Postoperative Quality of Life in Patients with Papillary Thyroid Cancer
Ju-Sung Kim
Journal of the Korea Academia-Industrial cooperation Society.2011; 12(3): 1260. CrossRef - Effects of Laughter Therapy on Depression, Quality of Life, Resilience and Immune Responses in Breast Cancer Survivors
Eun A Cho, Hyun Ei Oh
Journal of Korean Academy of Nursing.2011; 41(3): 285. CrossRef - Analysis of Nursing Intervention Studies on Patients with Breast Cancer in Korea
Kyung Sook Choi, Mi Sook Kim, In Ja Lee, Sang Young Han, Jung Ae Park, Joohyun Lee
Journal of Korean Oncology Nursing.2011; 11(1): 74. CrossRef
- Prediction Model for Postoperative Quality of Life Among Breast Cancer Survivors Along the Survivorship Trajectory From Pretreatment to 5 Years: Machine Learning–Based Analysis
- 1,523 View
- 9 Download
- 37 Crossref

- Effects of a Cognitive-Behavioral Nursing Intervention on Anxiety and Depression in Women with Breast Cancer undergoing Radiotherapy
- Myung-Sook Yoo, Haejung Lee, Jung-A Yoon
- J Korean Acad Nurs 2009;39(2):157-165. Published online April 28, 2009
- DOI: https://doi.org/10.4040/jkan.2009.39.2.157
-
 Abstract
Abstract
 PDF
PDF Purpose The purpose of this study was to analyze the effects of a cognitive-behavioral nursing intervention on anxiety and depression of patients with breast cancer undergoing radiotherapy.
Methods A nonequivalent control group design was used for the study. The research participants were patients with breast cancer (N=71; experimental group=35, comparison group=36) who received radiotherapy at P university hospital. The experimental group received a 6-week cognitive-behavioral nursing intervention (2 hr/week), which included nursing counseling, education about treatment choices for breast cancer and possible side effects and management strategies during radiotherapy, and rehabilitation exercise.
Results Following the intervention, the experimental group showed significantly lower levels of anxiety (Experimental group=34.60±6.35, Comparison group=44.63±9.93, t=3.552,
p <.001) and depression (Experimental group=10.20±6.61, Comparison group=17.81±10.85, t=3.542,p <.001) than the comparison group.Conclusion The findings from this study showed that cognitive-behavioral counseling applied by nurses is very effective to reduce anxiety and depression among patients with breast cancer. Therefore, providing nursing counseling to broader spectrum of patients with cancer should be considered. Further research would warrant future clinical application of nursing counseling.
-
Citations
Citations to this article as recorded by- Impact of combining cognitive intervention and psychological care on the mental health of patients with benign breast tumors
Feifei Xu, Sheng Xu
Psycho-Oncologie.2025;[Epub] CrossRef - Effects of specialized nursing intervention based on quantitative assessment strategy on psychological state and quality of life of patients with senile dementia
Angel Yong, Ying Zhao, Hai’e Xu, Qian Liu, Chuanying Huang
Acta Neurologica Belgica.2023; 123(6): 2213. CrossRef - Effects of Psychosocial Interventions for Patients with Breast Cancer: A Meta-analysis
Kyu-Sic Hwang, Kuy-Haeng Lee, Chan-Mo Yang, Hye-Jin Lee, Sang-Yeol Lee
Clinical Psychopharmacology and Neuroscience.2023; 21(1): 118. CrossRef - Nursing strategies to support psychological adaptation in adult cancer patients: a scoping review
Tiago André dos Santos Martins Peixoto, Nuno Miguel dos Santos Martins Peixoto, Cândida Assunção Santos Pinto, Célia Samarina Vilaça de Brito Santos
Revista da Escola de Enfermagem da USP.2021;[Epub] CrossRef - Function of a Psychological Nursing Intervention on Depression, Anxiety, and Quality of Life in Older Adult Patients With Osteoporotic Fracture
Liying Huang, Caiting Zhang, Jiahui Xu, Wei Wang, Miao Yu, Fusong Jiang, Liang Yan, Fanghui Dong
Worldviews on Evidence-Based Nursing.2021; 18(4): 290. CrossRef - Factors related to CPR performance ability of dental hygenists working in dental hospitals
Eun-Young Choi, Choong-Ho Choi
Journal of Korean Academy of Oral Health.2020; 44(4): 228. CrossRef - Non-pharmacological therapies for depressive symptoms in breast cancer patients: Systematic review and meta-analysis of randomized clinical trials
Liliana Coutiño-Escamilla, Maricela Piña-Pozas, Aurelio Tobías Garces, Brenda Gamboa-Loira, Lizbeth López-Carrillo
The Breast.2019; 44: 135. CrossRef - A psychological intervention programme for patients with breast cancer under chemotherapy and at a high risk of depression: A randomised clinical trial
Yeon Hee Kim, Kyung Sook Choi, Kihye Han, Hae Won Kim
Journal of Clinical Nursing.2018; 27(3-4): 572. CrossRef - A Study on Genetic Knowledge and Anxiety in Patients with Breast Cancer
Hyeyeon Seo, Myungsun Yi
Asian Oncology Nursing.2017; 17(3): 151. CrossRef - Health Promoting Behavior and Influencing Factors in Iranian Breast Cancer Survivors
Fatemeh Moghaddam Tabrizi
Asian Pacific Journal of Cancer Prevention.2015; 16(5): 1729. CrossRef - An Integrative Review of Depression Related to Intervention Studies for Women in Korea Journals
Eun Young Choi, Eun Hee Lee, Hye Jin Hyun, Mi Kyeong Byeon
Korean Journal of Women Health Nursing.2015; 21(4): 284. CrossRef - Psychosocial outcomes of e‐feedback of radiotherapy for breast cancer patients: a randomized controlled trial
Mervi Siekkinen, Seppo Pyrhönen, Anne Ryhänen, Tero Vahlberg, Helena Leino‐Kilpi
Psycho-Oncology.2015; 24(5): 515. CrossRef - A clinical randomized controlled trial of music therapy and progressive muscle relaxation training in female breast cancer patients after radical mastectomy: Results on depression, anxiety and length of hospital stay
Kaina Zhou, Xiaomei Li, Jin Li, Miao Liu, Shaonong Dang, Duolao Wang, Xia Xin
European Journal of Oncology Nursing.2015; 19(1): 54. CrossRef - Avaliação da intervenção cognitivo-comportamental em gestão do stress em pacientes com fadiga oncológica, em radioterapia
Cláudia Ng Deep, Isabel Leal, Ivone Patrão
Saúde e Sociedade.2014; 23(1): 293. CrossRef - Factors Affecting Sexual Function of Breast Cancer Women After Receiving Cancer Treatment
Hye Sun Byun, Bok Yae Chung, Gyung Duck Kim, Kyung Hae Kim, Eun Hee Choi
Asian Oncology Nursing.2013; 13(2): 85. CrossRef - Factors influencing health-promoting behaviors in Korean breast cancer survivors
Myungsun Yi, Jeongeun Kim
European Journal of Oncology Nursing.2013; 17(2): 138. CrossRef - Effects of a Simulation-based Educational Program for Gastroendoscopic Surgery Patients
Su Young Kwon, Jia Lee
Korean Journal of Adult Nursing.2013; 25(5): 494. CrossRef - Impacts of Fatigue, Pain, Anxiety, and Depression on the Quality of Life in Patients with Breast Cancer
Hye Sun Byun, Gyung Duck Kim
Asian Oncology Nursing.2012; 12(1): 27. CrossRef - Effects of a Nurse-Led Cognitive-Behavior Therapy on Fatigue and Quality of Life of Patients With Breast Cancer Undergoing Radiotherapy
Haejung Lee, Yeonjung Lim, Myung-Sook Yoo, Yongsuk Kim
Cancer Nursing.2011; 34(6): E22. CrossRef
- Impact of combining cognitive intervention and psychological care on the mental health of patients with benign breast tumors
- 1,569 View
- 28 Download
- 19 Crossref

 KSNS
KSNS
 E-SUBMISSION
E-SUBMISSION

 First
First Prev
Prev