Articles
- Page Path
- HOME > J Korean Acad Nurs > Volume 42(5); 2012 > Article
-
Original Article
- Development and Effectiveness of a Drug Dosage Calculation Training Program using Cognitive Loading Theory based on Smartphone Application
- Myoung Soo Kim1, Jung Ha Park1, Kyung-Yeon Park2
-
Journal of Korean Academy of Nursing 2012;42(5):689-698.
DOI: https://doi.org/10.4040/jkan.2012.42.5.689
Published online: October 12, 2012
1Department of Nursing, Pukyong National University, Busan, Korea
2Department of Nursing, Silla University, Busan, Korea
1Department of Nursing, Pukyong National University, Busan, Korea
2Department of Nursing, Silla University, Busan, Korea
- Address reprint requests to : Kim, Myoung Soo Department of Nursing, Pukyong National University, 599-1 Daeyeon 3-dong, Nam-gu, Busan 608-737, Korea Tel: +82-51-629-5782 Fax: +82-51-629-7906 E-mail: kanosa@pknu.ac.kr
Copyright © 2012 Korean Society of Nursing Science
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 1,863 Views
- 17 Download
- 25 Crossref
Figure & Data
REFERENCES
Citations

- Challenges in educating nursing students on mechanical ventilation: the case for interactive mobile learning tools – a randomized controlled trial
Alireza Samimi Sarangi, Kolsoum Deldar, Ahmad Bagheri Moghaddam, Razieh Froutan
BMC Nursing.2026;[Epub] CrossRef - Development and effectiveness of a smartphone-based serious game for disaster casualty triage training among nursing students in South Korea
Jieun Lee, Eunjoo Lee
Nurse Education in Practice.2026; 93: 104826. CrossRef - Development and effectiveness of online teaching on practical skills among nursing students: A systematic review and meta-analysis
Afang Li, Norhasmah Mohd Zain, Azlina Yusuf, Haiyan Deng, Qi He
Nurse Education in Practice.2024; 78: 103988. CrossRef - Development and Effectiveness of a Clinical Decision Support System for Pressure Ulcer Prevention Care Using Machine Learning
Myoung Soo Kim, Jung Mi Ryu, Byung Kwan Choi
CIN: Computers, Informatics, Nursing.2023; 41(4): 236. CrossRef - Effectiveness of a virtual reality application‐based education programme on patient safety management for nursing students: A pre‐test–post‐test study
Jae Woo Oh, Ji Eun Kim
Nursing Open.2023; 10(12): 7622. CrossRef - The Effect of Game-Based Clinical Nursing Skills Mobile Application on Nursing Students
Donghee Suh, Hyekyung Kim, Eunyoung E. Suh, Hyunsun Kim
CIN: Computers, Informatics, Nursing.2022; 40(11): 769. CrossRef - The effect of case-based learning based on flipped learning for nursing students
Min Hee Lee, Myung Sook Park
The Journal of Korean Academic Society of Nursing Education.2021; 27(2): 107. CrossRef - Smartphone distraction during nursing care: Systematic literature review
Massimo Fiorinelli, Sofia Di Mario, Antonella Surace, Micol Mattei, Carla Russo, Giulia Villa, Sara Dionisi, Emanuele Di Simone, Noemi Giannetta, Marco Di Muzio
Applied Nursing Research.2021; 58: 151405. CrossRef - A systematic review into the assessment of medical apps: motivations, challenges, recommendations and methodological aspect
A. H. Alamoodi, Salem Garfan, B. B. Zaidan, A. A. Zaidan, Moceheb Lazam Shuwandy, Mussab Alaa, M. A. Alsalem, Ali Mohammed, A. M. Aleesa, O. S. Albahri, Ward Ahmed Al-Hussein, O. R. Alobaidi
Health and Technology.2020; 10(5): 1045. CrossRef - Development and Utilization of a Clinical Decision Support System Contents for Pressure Ulcer Prevention Care
Myoung Soo Kim, Jung Mi Ryu
Journal of Health Informatics and Statistics.2020; 45(4): 365. CrossRef - The Effect of Cell Phones on Attention and Learning in Nursing Students
Lorena Gutiérrez-Puertas, Verónica V. Márquez-Hernández, Vanesa Gutiérrez-Puertas, Genoveva Granados-Gámez, Gabriel Aguilera-Manrique
CIN: Computers, Informatics, Nursing.2020; 38(8): 408. CrossRef - Using Video Feedback Through Smartphone Instant Messaging in Fundamental Nursing Skills Teaching: Observational Study
Xiaoxian Yang, Ri-Hua Xie, Si Chen, Wei Yu, Yan Liao, Daniel Krewski, Shi Wu Wen
JMIR mHealth and uHealth.2019; 7(9): e15386. CrossRef - Effects of Smartphone-Based Mobile Learning in Nursing Education: A Systematic Review and Meta-analysis
Ju Hee Kim, Hanjong Park
Asian Nursing Research.2019; 13(1): 20. CrossRef - Development and Evaluation of “Chronic Illness Care Smartphone Apps” on Nursing Students’ Knowledge, Self-efficacy, and Learning Experience
Jiyoung Kang, Eunyoung E. Suh
CIN: Computers, Informatics, Nursing.2018; 36(11): 550. CrossRef - Mobile Technology in Undergraduate Nursing Education: A Systematic Review
Hyejung Lee, Haeyoung Min, Su-mi Oh, Kaka Shim
Healthcare Informatics Research.2018; 24(2): 97. CrossRef - The Relationship Between Acceptance Intention Toward a Smartphone Healthcare Application and Health-Promoting Behaviors Among Nursing Students
Eun-Jin Choi, Se-Won Kang
CIN: Computers, Informatics, Nursing.2018; 36(10): 494. CrossRef - The Effects of an Interactive Nursing Skills Mobile Application on Nursing Students' Knowledge, Self-efficacy, and Skills Performance: A Randomized Controlled Trial
Hyunsun Kim, Eunyoung E. Suh
Asian Nursing Research.2018; 12(1): 17. CrossRef - Outcomes of a Drug Dosage Calculation Training Smartphone App on Learning Achievement, Metacognition, and Flow State According to Prior Knowledge
Kyung Yeon Park, Myoung Soo Kim
EURASIA Journal of Mathematics, Science and Technology Education.2018;[Epub] CrossRef - Development and Cross-cultural Validation of the Korean Version of SMArtphone’s uSability Heuristics (SMASH)
Yeo Won Jeong, Jung A Kim
Healthcare Informatics Research.2017; 23(4): 328. CrossRef - The Effects of Smartphone Application to Educate Patient on Patient Safety in Hospitalized Surgical Patients
Hyo Jin Choi, Eunjoo Lee
Korean Journal of Adult Nursing.2017; 29(2): 154. CrossRef - Use of mobile devices and medication errors in acute care
Nicole Harder, Jannell Plouffe, Diane Cepanec, Kari Mann, Mê-Linh Lê, Patricia Gregory, Patrick Griffith, Kathy Doerksen
JBI Database of Systematic Reviews and Implementation Reports.2016; 14(9): 47. CrossRef - Development of a Smartphone Application for Clinical Decision Making of Medication Administration
Myoung-Soo Kim, Jung-Ha Park, Sungmin Kim
Journal of the Korea Academia-Industrial cooperation Society.2014; 15(3): 1650. CrossRef - Predictors of Drug Dosage Calculation Error Risk in Newly Graduated Nurses
Myoung Soo Kim, Jung Soon Kim, Won Choon Ha
Journal of Korean Biological Nursing Science.2014; 16(2): 113. CrossRef - Development and Effectiveness of Smartphone Application for the Medication Confirmation of High-alert Medications
Myoung Soo Kim
Korean Journal of Adult Nursing.2014; 26(3): 253. CrossRef - The Mediating Effect of Drug Calculation Confidence in the Relationship between Interest in Medication and Drug Calculation Competency
Hyoung Sook Park, Gyoo Yeong Cho, Dong-Hee Kim, Sang Hee Kim, Myoung Soo Kim
Journal of Korean Biological Nursing Science.2013; 15(4): 155. CrossRef
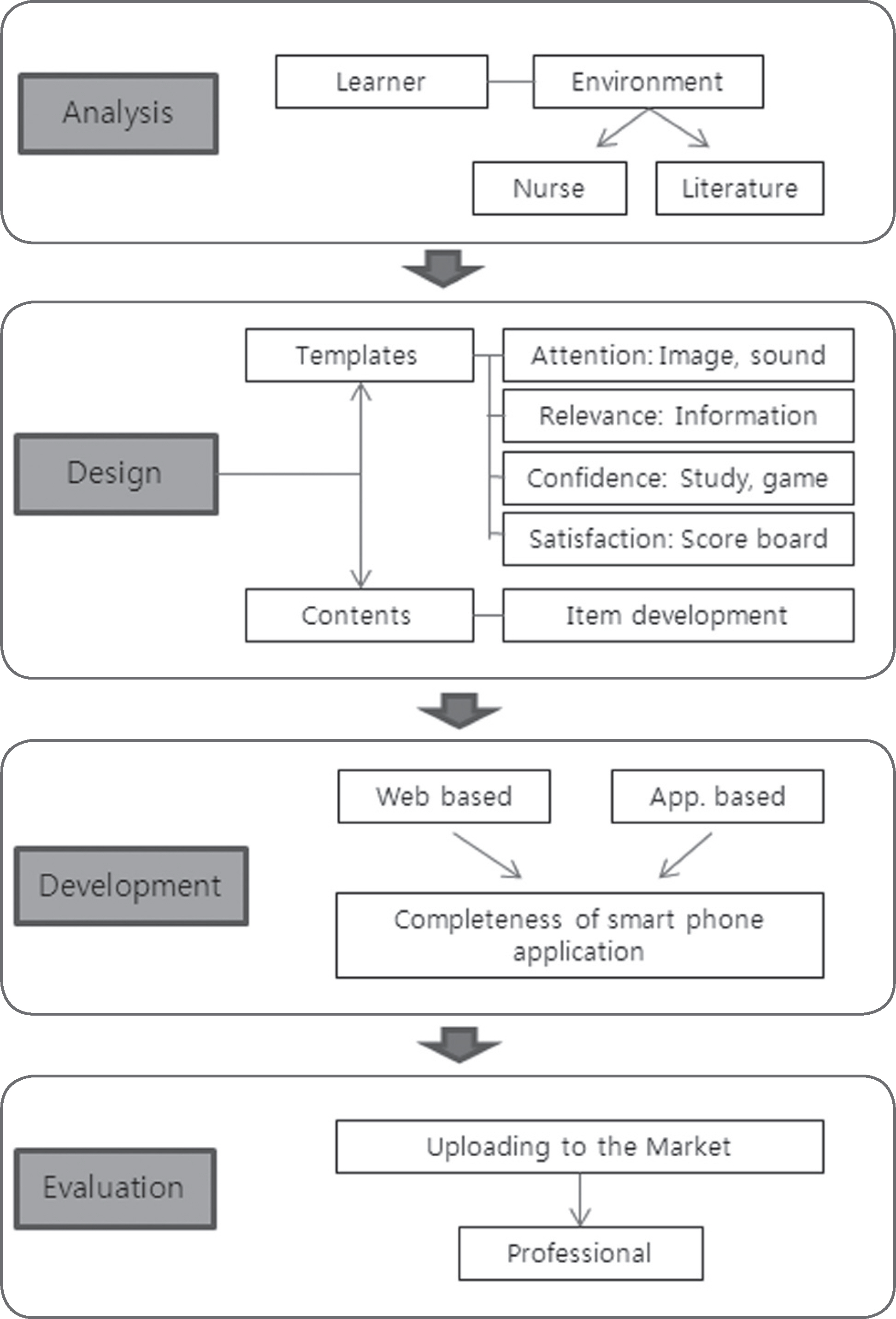

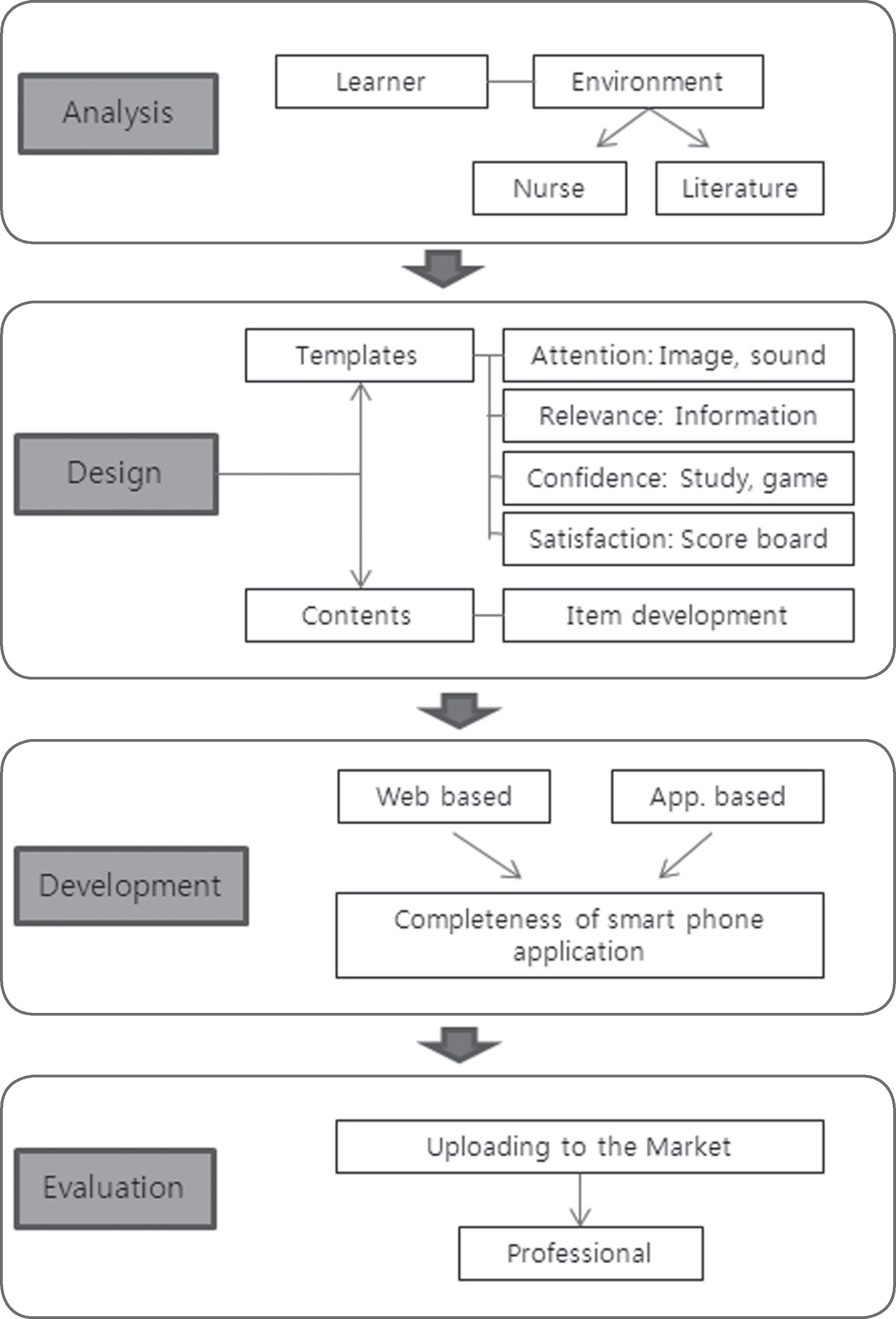
Figure 1.
Figure 2.
| Principles of the application development | |
|---|---|
| Teaching strategies for reducing cognitive loading | Construction strategies for smartphone based application development |
| Goal-free effect | Construct the learning area and the gaming area. Doesn't display the aim of the lesson in the learning area. |
| Worked example effect | Insert the example tabs on the introduction page in the learning area, which provide solved examples. |
| Completion problem effect | Provide the tips, but make participants write the answers themselves. |
| Split attention effect | Arrange all contents in one page which prevents scrolling to see the cut screen. |
| Variability practice effect | Construct gaming area in order to help participants solve the questionnaires repeatedly. |
| Modality effect | Provide the screen changes and auditory stimulations at the period of scoring. |
| Redundancy effect | Construct the standardized form of questionnaire to prevent cognitive loading resulting from the various information sources. |
| Multi-media effect | Use visual stimuli and auditorial stimuli with graphs, illustrations and audio clips. |
| Examples of the questionnaires | |
| Metric conversion | Convert 1.17 g to mg. |
| Tablet calculation | 62.5 mcg of digoxin is prescribed daily. On hand you have 250 mcg tablets. How many tablets will you give? |
| Fluid dosage calculation | 0.75 g of lincomycin hydrochloride IV 8-12 hourly is prescribed. On hand you have 300 mg in 2 mL. How many mL will you administer? |
| Drop rate calculation | 1 L of Lactated Ringer's solution is prescribed over 10 hours. The drop factor is 15. What is the drip rate (drops/minute) required? |
| Variables | Categories (Numbers of items) | Exp. (n=37) | Cont. (n=41) | t/χ2 (p) |
|---|---|---|---|---|
| n (%) or M±SD | ||||
| Age (year) | 20.30±1.51 | 20.15±1.28 | 0.48 (.633) | |
| Gender* | Female | 36 (97.3) | 37 (90.2) | (.362) |
| Male | 1 (0.7) | 4 (9.8) | ||
| Self-efficacy for drug dosage calculation | Confidence for mathematics (6) | 3.30±0.66 | 3.09±0.79 | 1.23 (.211) |
| Confidence for drug dosage calculation (7) | 2.98±0.72 | 2.71±0.75 | 1.64 (.106) | |
| Total (13) | 3.13±0.62 | 2.89±0.72 | 1.58 (.119) | |
| Anxiety for drug dosage calculation | Fear of asking help (4) | 2.97±0.52 | 3.01±0.69 | −0.24 (.812) |
| Self-concept (7) Total (11) | 2.11±0.67 2.42 0.50 | 2.60±0.93 2.75 0.67 | −2.66 (.010) 2.41 (.018) | |
| Total (11) | 2.42±0.50 | 2.75±0.67 | −2.41 (.018) | |
| Calculation ability | Metric conversion (3) | 2.27±0.87 | 1.98±0.69 | 1.67 (.100) |
| Tablet dosage calculation (3) | 0.95±0.23 | 1.07±0.41 | −1.66 (.101) | |
| Fluid amount calculation (3) | 2.76±0.72 | 2.63±0.80 | 0.71 (.481) | |
| Drop rate calculation (3) | 1.43±1.07 | 1.10±0.92 | 1.48 (.144) | |
| Total (12) | 7.40±2.18 | 6.78±1.59 | 1.43 (.156) | |
| Variables | Categories | Exp. (n=37) | Cont. (n=41) | t or F (p) |
|---|---|---|---|---|
| M±SD | M±SD | |||
| Self-efficacy for drug dosage | Confidence for mathematics | 3.48±0.60 | 3.15±0.75 | 2.15 (.035) |
| calculation | Confidence for drug dosage calculation | 3.66±0.64 | 2.95±0.77 | 4.45 (<.001) |
| Total | 3.58±0.57 | 3.04±0.67 | 3.82 (<.001) | |
| Anxiety for drug dosage | Fear of asking help | 3.02±0.67 | 2.90±0.65 | 0.79 (.433) |
| calculation | Self-concept* | 2.14±0.65 | 2.51±0.69 | 0.82 (.684) |
| Total* | 2.46±0.49 | 2.65±0.43 | 0.66 (.862) | |
| Calculation ability | Metric conversion | 2.19±0.91 | 1.78±0.69 | 2.25 (.027) |
| Tablet dosage calculation | 2.54±0.77 | 2.12±0.90 | 2.20 (.031) | |
| Fluid amount calculation | 2.81±0.57 | 2.63±0.70 | 1.23 (.223) | |
| Drop rate calculation | 2.41±0.80 | 1.41±1.09 | 4.60 (<.001) | |
| Total | 9.95±2.31 | 7.95±2.12 | 3.98 (<.001) | |
| Satisfaction for program | Effective way to learn | 4.38±0.72 | − | − |
| Generally appropriate | 4.30±0.57 | − | − | |
| Recommendable | 4.24±0.55 | − | − | |
| Frequency | Visit to learning area (number/week) | 5.45±7.10 | − | − |
| Visit to game area (number/week) | 7.68±10.26 | − | − | |
| Connect hours (min/week) | 21.93±26.61 | − | − |
Exp.=Experimental group; Cont.=Control group. *Fisher's exact test.
Exp.=Experimental group; Cont.=Control group. *ANCOVAs were used to identify group differences at post-test.
 KSNS
KSNS
 Submit an article
Submit an article

 Cite
Cite