Articles
- Page Path
- HOME > J Korean Acad Nurs > Volume 44(4); 2014 > Article
-
Original Article
- Effects of a Progressive Walking Program on Physical Activity, Exercise Tolerance, Recovery, and Post-Operative Complications in Patients with a Lung Resection
- Inah Kim, Haejung Lee
-
Journal of Korean Academy of Nursing 2014;44(4):381-390.
DOI: https://doi.org/10.4040/jkan.2014.44.4.381
Published online: August 15, 2014
College of Nursing, Pusan National University, Yangsan, Korea
College of Nursing, Pusan National University, Yangsan, Korea
- Address reprint requests to : Lee, Haejung College of Nursing, Pusan National University, Beomeo-ri, Mulgeum-eup, Yangsan 626-870, Korea Tel: +82-51-510-8344 Fax: +82-51-510-8308 E-mail: haejung@pusan.ac.kr
Copyright © 2014 Korean Society of Nursing Science
This is an Open Access article distributed under the terms of the Creative Commons Attribution NoDerivs License. (http://creativecommons.org/licenses/by-nd/4.0) If the original work is properly cited and retained without any modification or reproduction, it can be used and re-distributed in any format and medium.
Abstract
-
Purpose
- The purpose of this study was to identify the effects of a Progressive Walking program (PW) on physical activity, exercise tolerance, recovery, and post-operative complications for patients with a lung resection.
-
Methods
- A nonequivalent control group non-synchronized design was utilized and 37 participants with a lung resection (22 for control group, 15 for experimental group) were recruited at A university hospital from December 2012 to August 2013. The PW consisted of preoperative education, goal setting, and feedback, provided to the experimental group, and usual care to the control group. Data were analyzed using the SPSS WIN 18.0.
-
Results
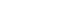
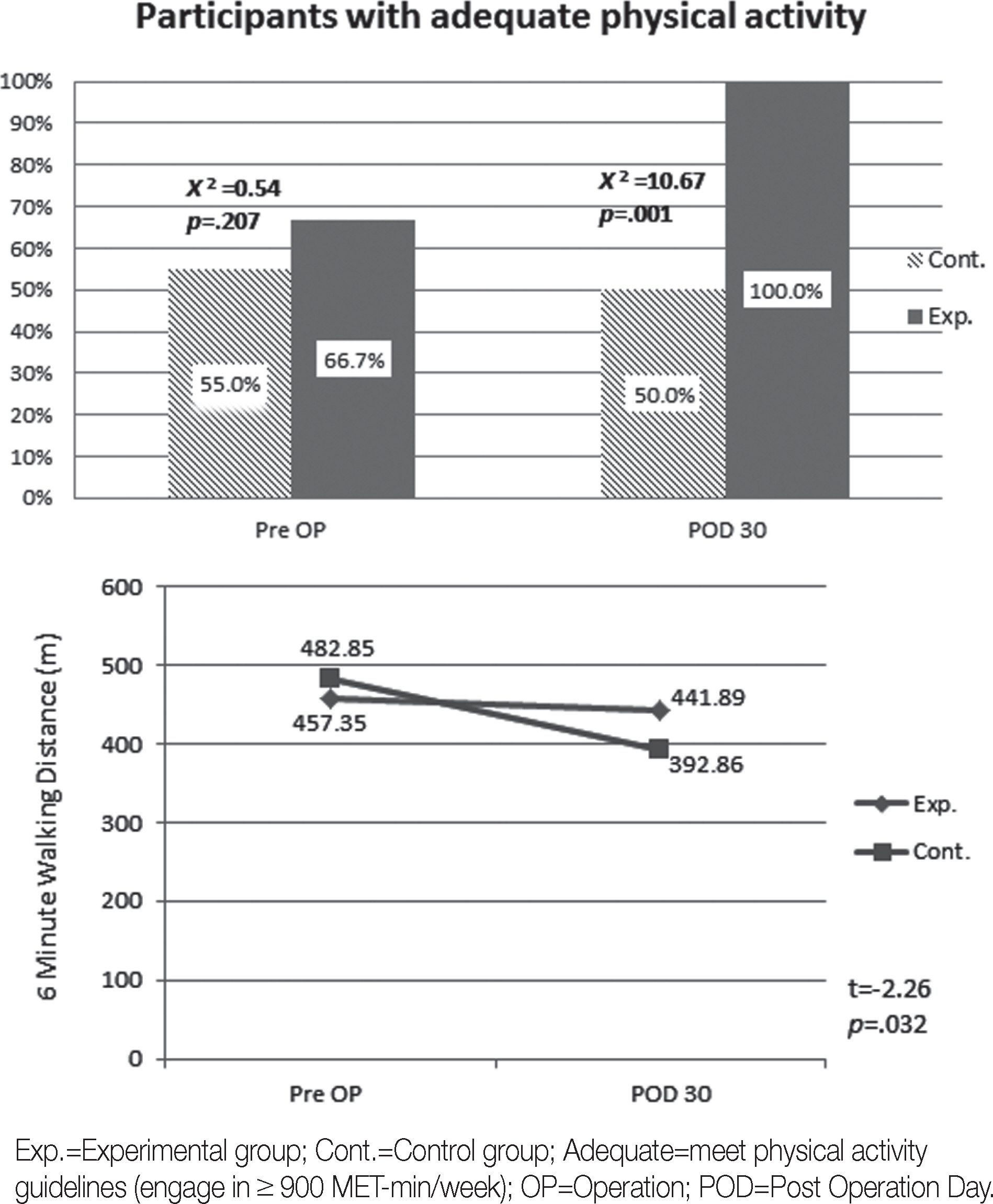
- A higher proportion of patients in the experimental group showed adequate levels of physical activity (p= .001), shorter period of chest tube retention (≤ 7 days; p= .011), and shorter stay in the hospital (≤ 10 days; p= .036) than patients in the control group. Patients in the experimental group reported longer 6-minute walking distance (p= .032) and lower levels of dyspnea (p= .049) than patients in the control group. The PW did not influence the occurrence of pulmonary complications.
-
Conclusion
- The findings of this study suggest that the PW could be a useful strategy for improving patients’ post-operative health and reducing cost after lung resection.
| Characteristics | Categories | Total | Exp. (n=15) | Cont. (n=22) | χ2 | p |
|---|---|---|---|---|---|---|
| n (%) or M±SD | n (%) or M±SD | n (%) or M±SD | ||||
| Age (year) | <65 | 25 (67.6) | 12 (80.0) | 13 (59.1) | .286* | |
| ≥65 | 12 (32.4) | 3 (20.0) | 9 (40.9) | |||
| 59.51±11.06 | 59.46±8.89 | 59.50±12.54 | ||||
| Gender | Male | 28 (75.7) | 11 (73.3) | 17 (77.3) | 1.000* | |
| Female | 9 (24.3) | 4 (26.7) | 5 (22.7) | |||
| Spouse | Yes No | 34 (91.9) 3 (8.1) | 14 (93.3) 1 (6.7) | 20 (90.9) 2 (9.1) | 1.000* | |
| Education | ≤Middle school | 19 (51.4) | 8 (53.3) | 11 (50.0) | 0.04 | 1.000 |
| ≥High school | 18 (48.6) | 7 (46.7) | 11 (50.0) | |||
| Regular exercise | Yes No | 14 (37.8) 23 (62.2) | 7 (46.7) 8 (53.3) | 7 (31.8) 15 (68.2) | 0.84 | .361 |
| Operation history | Yes | 20 (54.1) | 8 (53.3) | 13 (59.1) | 0.55 | .457 |
| No | 17 (45.9) | 7 (46.7) | 9 (40.9) | |||
| BMI | <18.5 | 1 (2.7) | 0 (0.0) | 1 (4.6) | .891* | |
| 18.5 to<25.0 | 30 (81.1) | 12 (80.0) | 18 (81.8) | |||
| ≥25.0 | 6 (16.2) | 3 (20.0) | 3 (13.6) | |||
| 23.01±2.73 | 23.08±2.96 | 22.96±2.63 | ||||
| Comorbidity | Yes | 25 (67.6) | 9 (60.0)† | 16 (27.3)‡ | 0.66 | .202 |
| No | 12 (32.4) | 6 (40.0) | 6 (72.7) | |||
| Smoking state | Never smoked | 22 (59.5) | 8 (53.3) | 14 (63.6) | .177* | |
| Quit smoking Current smoker | 9 (24.3) 6 (16.2) | 1 (6.7) 6 (40.0) | 3 (13.7) 5 (22.7) | |||
| FEV1 % predicted | <80 | 27 (73.0) | 10 (66.7) | 17 (77.3) | 0.51 | .708 |
| ≥80 | 10 (27.0) | 5 (33.3) | 5 (22.7) | |||
| 72.70±9.97 | 73.00±9.97 | 72.50±10.19 |
| Outcome variables | Exp. (n=15) | Cont. (n=22) | t | p |
|---|---|---|---|---|
| n (%) or M±SD | n (%) or M±SD | |||
| Total steps at POD 30 days | 9,933.33±6,485.85 | − | ||
| <10,000 | 8 (53.3) | − | ||
| ≥10,000 | 7 (46.7) | − | ||
| Recovery | ||||
| Number of days with chest tube retention (days) | 5.93±2.93 | 8.45±6.20 | .016* | |
| ≤7 | 13 (86.7) | 10 (45.5) | ||
| >7† | 2 (13.3) | 12 (54.5) | ||
| Hospital stay (days) | 8.80±3.73 | 11.68±6.46 | .047* | |
| ≤10 | 12 (80.0) | 10 (45.5) | ||
| >10‡ | 3 (20.0) | 12 (54.5) | ||
| Dyspnea | 12.59±11.00 | 21.71±16.25 | 2.03 | .049 |
| Occurrence of pulmonary complication (OP day-POD 30) | 0 (0.0) | 3 (13.6) | .233* |
Exp.=Experimental group; Cont.=Control group; OP=Operation; POD=Post operative Day; *Fisher’s exact test;
†Reasons=Persistent air leakage (43.0%), chest tube drainage>100 ml for last 24 hours (28.5%), both persistent air leak and chest tube drainage>100 ml for last 24 hours (28.5%);
‡Reasons=Further evaluation (40.0%), delayed removal of chest tube (33.3%), refuse to be discharged (20.0%), pneumonia (6.7%).
- 1. Statistics Korea. 2010 life tables for Korea [Internet]. Daejeon: Author; 2011.[cited 2012 December 10]. Available from:. http://kostat.go.kr/portal/korea/kor_nw/3/index.board?bmode=read&aSeq=252533
- 2. Win T, Groves AM, Ritchie AJ, Wells FC, Cafferty F, Laroche CM. The effect of lung resection on pulmonary function and exercise capacity in lung cancer patients. Respiratory Care. 2007;52(6):720–726.ArticlePubMedPDF
- 3. Johar RS, Hayn MH, Stegemann AP, Ahmed K, Agarwal P, Balbay MD, et al. Complications after robot-assisted radical cystectomy: Results from the International Robotic Cystectomy Consortium. European Urology. 2013;64(1):52–57. http://dx.doi.org/10.1016/j.eururo.2013.01.010ArticlePubMed
- 4. Scholes RL, Browning L, Sztendur EM, Denehy L. Duration of anaesthesia, type of surgery, respiratory co-morbidity, predicted VO2max and smoking predict postoperative pulmonary complications after upper abdominal surgery: An observational study. Australian Journal of Physiotherapy. 2009;55(3):191–198.ArticlePubMed
- 5. Agostini P, Cieslik H, Rathinam S, Bishay E, Kalkat MS, Rajesh PB, et al. Postoperative pulmonary complications following thoracic surgery: Are there any modifiable risk factors? Thorax. 2010;65(9):815–818. http://dx.doi.org/10.1136/thx.2009.123083ArticlePubMed
- 6. Varela G, Ballesteros E, Jiménez MF, Novoa N, Aranda JL. Cost-effectiveness analysis of prophylactic respiratory physiotherapy in pulmonary lobectomy. European Journal of Cardio-Thoracic Surgery. 2006;29(2):216–220. http://dx.doi.org/10.1016/j.ejcts.2005.11.002ArticlePubMed
- 7. Novoa N, Ballesteros E, Jimenez MF, Aranda JL, Varela G. Chest physiotherapy revisited: Evaluation of its influence on the pulmonary morbidity after pulmonary resection. European Journal of Cardio-Thoracic Surgery. 2011;40(1):130–134. http://dx.doi.org/10.1016/j.ejcts.2010.11.028ArticlePubMed
- 8. Cesario A, Ferri L, Galetta D, Pasqua F, Bonassi S, Clini E, et al. Post-operative respiratory rehabilitation after lung resection for non-small cell lung cancer. Lung Cancer. 2007;57(2):175–180. http://dx.doi.org/10.1016/j.lungcan.2007.02.017ArticlePubMed
- 9. Hirschhorn AD, Richards D, Mungovan SF, Morris NR, Adams L. Supervised moderate intensity exercise improves distance walked at hospital discharge following coronary artery bypass graft surgery: A ran- domised controlled trial. Heart, Lung & Circulation. 2008;17(2):129–138. http://dx.doi.org/10.1016/j.hlc.2007.09.004Article
- 10. Souza Possa S, Braga Amador C, Meira Costa A, Takahama Sakamoto E, Seiko Kondo C, Maida Vasconcellos AL, et al. Implementation of a guideline for physical therapy in the postoperative period of upper abdominal surgery reduces the incidence of atelectasis and length of hospital stay. Revista Portuguesa de Pneumologia. 2014;20(2):69–77. http://dx.doi.org/10.1016/j.rppneu.2013.07.005ArticlePubMed
- 11. Reeve JC, Nicol K, Stiller K, McPherson KM, Denehy L. Does physiotherapy reduce the incidence of postoperative complications in patients following pulmonary resection via thoracotomy? A protocol for a randomised controlled trial. Journal of Cardiothoracic Surgery. 2008;3:48http://dx.doi.org/10.1186/1749-8090-3-48ArticlePubMedPMCPDF
- 12. Arbane G, Tropman D, Jackson D, Garrod R. Evaluation of an early exercise intervention after thoracotomy for non-small cell lung cancer (NSCLC), effects on quality of life, muscle strength and exercise tolerance: Randomised controlled trial. Lung Cancer. 2011;71(2):229–234. http://dx.doi.org/10.1016/j.lungcan.2010.04.025ArticlePubMed
- 13. Seo YH, Kang HS. The effects of the respiration strengthening exercise program on pulmonary function, anxiety, and sleep of patients underwent lung surgery. Clinical Nursing Research. 2007;13(3):157–167.
- 14. Jung KJ, Lee YS. The effect of a breathing exercise intervention on pulmonary function after lung lobectomy. Journal of Korean Oncology Nursing. 2010;10(1):95–102.
- 15. Hong YL. Effect of preoperative educational DVD on postoperative self care knowledge and performance in lung cancer patient [master’s thesis]. Seoul: Hanyang University; 2007.
- 16. Bourke L, Homer KE, Thaha MA, Steed L, Rosario DJ, Robb KA, et al. Interventions for promoting habitual exercise in people living with and beyond cancer. Cochrane Database of Systematic Reviews. 2013;9:CD010192http://dx.doi.org/10.1002/14651858.CD010192.pub2Article
- 17. Lyons EJ, Hatkevich C. Prevalence of behavior changing strategies in fitness video games: Theory-based content analysis. Journal of Medical Internet Research. 2013;15(5):e81http://dx.doi.org/10.2196/jmir.2403ArticlePubMedPMC
- 18. Richardson CR, Newton TL, Abraham JJ, Sen A, Jimbo M, Swartz AM. A meta-analysis of pedometer-based walking interventions and weight loss. Annals of Family Medicine. 2008;6(1):69–77.ArticlePubMedPMC
- 19. Oh JY, Yang YJ, Kim BS, Kang JH. Validity and reliability of Korean version of international physical activity questionnaire (IPAQ) short form. Journal of the Korean Academy of Family Medicine. 2007;28(7):532–541.
- 20. Haskell WL, Lee IM, Pate RR, Powell KE, Blair SN, Franklin BA, et al. Physical activity and public health: Updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Circulation. 2007;116(9):1081–1093. http://dx.doi.org/10.1161/circulationaha.107.185649ArticlePubMed
- 21. Rikli RE, Jones J. The reliability and validity of a 6-minute walk test as a measure of physical endurance in older adults. Journal of Aging and Physical Activity. 1988;6(4):363–375.Article
- 22. ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: Guidelines for the six-minute walk test. American Journal of Respiratory and Critical Care Medicine. 2002;166(1):111–117. http://dx.doi.org/10.1164/ajrccm.166.1.at1102ArticlePubMedPDF
- 23. Roh JS. Development of critical pathway for patients with lobectomy and pneumonectomy [master’s thesis]. Seoul: Yonsei University; 2003.
- 24. Chie WC, Yang CH, Hsu C, Yang PC. Quality of life of lung cancer patients: Validation of the Taiwan Chinese version of the EORTC QLQ-C30 and QLQ-LC13. Quality of Life Research. 2004;13(1):257–262.ArticlePubMed
- 25. Novoa N, Varela G, Jiménez MF, Aranda JL. Influence of major pulmonary resection on postoperative daily ambulatory activity of the patients. Interactive Cardiovascular and Thoracic Surgery. 2009;9(6):934–938. http://dx.doi.org/10.1510/icvts.2009.212332ArticlePubMed
- 26. Coups EJ, Park BJ, Feinstein MB, Steingart RM, Egleston BL, Wilson DJ, et al. Correlates of physical activity among lung cancer survivors. Psycho-Oncology.. 2009;18(4):395–404. http://dx.doi.org/10.1002/pon.1520ArticlePubMedPMC
- 27. Kervio G, Carre F, Ville NS. Reliability and intensity of the six-minute walk test in healthy elderly subjects. Medicine and Science in Sports and Exercise. 2003;35(1):169–174. http://dx.doi.org/10.1249/01.mss.0000043545.02712.a7ArticlePubMed
- 28. Nimmo MA, Leggate M, Viana JL, King JA. The effect of physical activity on mediators of inflammation. Diabetes, Obesity & Metabolism. 2013;15(Suppl 3):51–60. http://dx.doi.org/10.1111/dom.12156Article
- 29. Brunelli A, Refai M, Xiume F, Salati M, Sciarra V, Socci L, et al. Performance at symptom-limited stair-climbing test is associated with increased cardiopulmonary complications, mortality, and costs after major lung resection. The Annals of Thoracic Surgery. 2008;86(1):240–247. http://dx.doi.org/10.1016/j.athoracsur.2008.03.025ArticlePubMed
- 30. Courneya KS, Friedenreich CM. Physical activity and cancer control. Seminars in Oncology Nursing. 2007;23(4):242–252. http://dx.doi.org/10.1016/j.soncn.2007.08.002ArticlePubMed
- 31. Chung CW, Lee S, Hwang SW, Park EH. Systematic review of exercise effects on health outcomes in women with breast cancer. Asian Nursing Research. 2013;7(3):149–159. http://dx.doi.org/10.1016/j.anr.2013.07.005ArticlePubMed
REFERENCES
Figure & Data
REFERENCES
Citations

- Effects of patient-based self-assessed fatigue intervention on early postoperative ambulation following gynaecological oncology surgery: a randomised controlled non-inferiority trial
Qian Du, Bo Chen, Xiaohong Zhang, Hong He, Xiaomin Qin, Lin Li, Junyi Du, Xindi He, Shaoyong Xu, Huang Xiaojie
BMJ Open.2024; 14(7): e078461. CrossRef - Walking to a better future? Postoperative ambulation after cesarean delivery and complications: A prospective study
Offra Engel, Einat Haikin Herzberger, Yael Yagur, Anat Hershko Klement, Ami Fishman, Naama Constantini, Tal Biron Shental
International Journal of Gynecology & Obstetrics.2022; 157(2): 391. CrossRef - Effectiveness of Exercise after Lung Cancer Surgery: A Systematic Review in PubMed Database
Ui Min Jerng
Journal of Korean Medicine Rehabilitation.2021; 31(1): 149. CrossRef - Applying Extended Theory of Planned Behavior for Lung Cancer Patients Undergone Pulmonary Resection: Effects on Self-Efficacy for Exercise, Physical Activities, Physical Function, and Quality of Life
Yeonjung Lim, Haejung Lee, Do Hyung Kim, Yeong Dae Kim
Journal of Korean Academy of Nursing.2020; 50(1): 66. CrossRef - Preoperative exercise training for patients with non-small cell lung cancer
Vinicius Cavalheri, Catherine Granger
Cochrane Database of Systematic Reviews.2017;[Epub] CrossRef - The Effects of a Standardized Preoperative Education Program on Stomach Cancer Patients undergoing Gastrectomy
Min Ah Yun, So Sun Kim, SangHee Kim, Sung Hoon Noh
Asian Oncology Nursing.2016; 16(2): 85. CrossRef
Figure 1.
Contents of Progressive Walking Program
| Categories | Contents |
|---|---|
| Pre operation education | 1) Preview=Exercise, manual for Pedometer. |
| 2) Video=Anatomy of lung, kind of operation, importance of exercise & nutrition. | |
| → Provided to patients and their family caregivers | |
| Goal setting | 1) Walking=Using the pedometer. |
| Start from 1000 steps and increase 8 % everyday. (POD 10=1999 steps/POD 20=4315 steps/POD 30=10062 steps) | |
| 2) Shoulder=Elevation through flexion & abduction, external & internal rotation (OP day=1 set). | |
| Once 1 set achieved, ↑the numbers of sets (Max 8 sets). 3) Respiration=Deep breathing & coughing (OP day=1 set). | |
| Once 1 set achieved, ↑the numbers of sets (Max 8 sets). | |
| Feedback | 1) Identify the amount of exercise & difficulties during exercise. |
| 2) Encouraging message=Address barriers to exercise for increasing amounts of exercise. POD 1-5=Provided daily feedback. | |
| POD 6-30=Provided feedback once every 3 days (Feedback by telephone call after discharge). |
POD=Post operative day; OP=Operation.
Homogeneity Test for Characteristics between Experimental and Control Group Participants (N=37)
| Characteristics | Categories | Total | Exp. (n=15) | Cont. (n=22) | χ2 | p |
|---|---|---|---|---|---|---|
| n (%) or M±SD | n (%) or M±SD | n (%) or M±SD | ||||
| Age (year) | <65 | 25 (67.6) | 12 (80.0) | 13 (59.1) | .286* | |
| ≥65 | 12 (32.4) | 3 (20.0) | 9 (40.9) | |||
| 59.51±11.06 | 59.46±8.89 | 59.50±12.54 | ||||
| Gender | Male | 28 (75.7) | 11 (73.3) | 17 (77.3) | 1.000* | |
| Female | 9 (24.3) | 4 (26.7) | 5 (22.7) | |||
| Spouse | Yes No | 34 (91.9) 3 (8.1) | 14 (93.3) 1 (6.7) | 20 (90.9) 2 (9.1) | 1.000* | |
| Education | ≤Middle school | 19 (51.4) | 8 (53.3) | 11 (50.0) | 0.04 | 1.000 |
| ≥High school | 18 (48.6) | 7 (46.7) | 11 (50.0) | |||
| Regular exercise | Yes No | 14 (37.8) 23 (62.2) | 7 (46.7) 8 (53.3) | 7 (31.8) 15 (68.2) | 0.84 | .361 |
| Operation history | Yes | 20 (54.1) | 8 (53.3) | 13 (59.1) | 0.55 | .457 |
| No | 17 (45.9) | 7 (46.7) | 9 (40.9) | |||
| BMI | <18.5 | 1 (2.7) | 0 (0.0) | 1 (4.6) | .891* | |
| 18.5 to<25.0 | 30 (81.1) | 12 (80.0) | 18 (81.8) | |||
| ≥25.0 | 6 (16.2) | 3 (20.0) | 3 (13.6) | |||
| 23.01±2.73 | 23.08±2.96 | 22.96±2.63 | ||||
| Comorbidity | Yes | 25 (67.6) | 9 (60.0) |
16 (27.3) |
0.66 | .202 |
| No | 12 (32.4) | 6 (40.0) | 6 (72.7) | |||
| Smoking state | Never smoked | 22 (59.5) | 8 (53.3) | 14 (63.6) | .177* | |
| Quit smoking Current smoker | 9 (24.3) 6 (16.2) | 1 (6.7) 6 (40.0) | 3 (13.7) 5 (22.7) | |||
| FEV1 % predicted | <80 | 27 (73.0) | 10 (66.7) | 17 (77.3) | 0.51 | .708 |
| ≥80 | 10 (27.0) | 5 (33.3) | 5 (22.7) | |||
| 72.70±9.97 | 73.00±9.97 | 72.50±10.19 |
Exp.=Experimental group; Cont.=Control group; FEV1=Forced Expiratory Volume in 1 second; BMI=Body Mass Index. *Fisher’s exact test;
†Hypertension, diabetes;
‡Hypertension, diabetes, arthritis, osteoporosis, gastritis.
Homogeneity Test for Levels of Physical Activity, 6 Minute Walk Distance, and Dyspnea at Pre-test between Experimental and Control Groups (N=37)
| Characteristics | Total | Exp. (n=15) | Cont. (n=22) | χ2 or t or U | p |
|---|---|---|---|---|---|
| n (%) or M±SD | n (%) or M±SD | n (%) or M±SD | |||
| Physical activity | 0.54 | .207 | |||
| Adequate | 22 (59.5) | 10 (66.7) | 12 (54.5) | ||
| Inadequate | 15 (40.5) | 5 (33.3) | 10 (45.5) | ||
| 6 minute walk distance (m) | 472.35±83.91 | 457.35±78.45 | 482.85±87.95 | −0.89 | .382 |
| Dyspnea | 12.01±13.45 | 10.37±9.82 | 13.13±15.58 | 160 | .870 |
Exp.=Experimental group; Cont.=Control group; Adequate=Meet physical activity guidelines (≥900 MET-min/wk); Inadequate=Do not meet physical activity guidelines (<900 MET-min/wk).
Effects of Progressive-walking Program on Daily Steps, Pulmonary Complications, and Recovery (N=37)
| Outcome variables | Exp. (n=15) | Cont. (n=22) | t | p |
|---|---|---|---|---|
| n (%) or M±SD | n (%) or M±SD | |||
| Total steps at POD 30 days | 9,933.33±6,485.85 | − | ||
| <10,000 | 8 (53.3) | − | ||
| ≥10,000 | 7 (46.7) | − | ||
| Recovery | ||||
| Number of days with chest tube retention (days) | 5.93±2.93 | 8.45±6.20 | .016* | |
| ≤7 | 13 (86.7) | 10 (45.5) | ||
| >7 |
2 (13.3) | 12 (54.5) | ||
| Hospital stay (days) | 8.80±3.73 | 11.68±6.46 | .047* | |
| ≤10 | 12 (80.0) | 10 (45.5) | ||
| >10 |
3 (20.0) | 12 (54.5) | ||
| Dyspnea | 12.59±11.00 | 21.71±16.25 | 2.03 | .049 |
| Occurrence of pulmonary complication (OP day-POD 30) | 0 (0.0) | 3 (13.6) | .233* |
Exp.=Experimental group; Cont.=Control group; OP=Operation; POD=Post operative Day; *Fisher’s exact test;
†Reasons=Persistent air leakage (43.0%), chest tube drainage>100 ml for last 24 hours (28.5%), both persistent air leak and chest tube drainage>100 ml for last 24 hours (28.5%);
‡Reasons=Further evaluation (40.0%), delayed removal of chest tube (33.3%), refuse to be discharged (20.0%), pneumonia (6.7%).
POD=Post operative day; OP=Operation.
Exp.=Experimental group; Cont.=Control group; FEV1=Forced Expiratory Volume in 1 second; BMI=Body Mass Index. *Fisher’s exact test; Hypertension, diabetes; Hypertension, diabetes, arthritis, osteoporosis, gastritis.
Exp.=Experimental group; Cont.=Control group; Adequate=Meet physical activity guidelines (≥900 MET-min/wk); Inadequate=Do not meet physical activity guidelines (<900 MET-min/wk).
Exp.=Experimental group; Cont.=Control group; OP=Operation; POD=Post operative Day; *Fisher’s exact test; Reasons=Persistent air leakage (43.0%), chest tube drainage>100 ml for last 24 hours (28.5%), both persistent air leak and chest tube drainage>100 ml for last 24 hours (28.5%); Reasons=Further evaluation (40.0%), delayed removal of chest tube (33.3%), refuse to be discharged (20.0%), pneumonia (6.7%).
 KSNS
KSNS
 Submit an article
Submit an article
 Cite
Cite